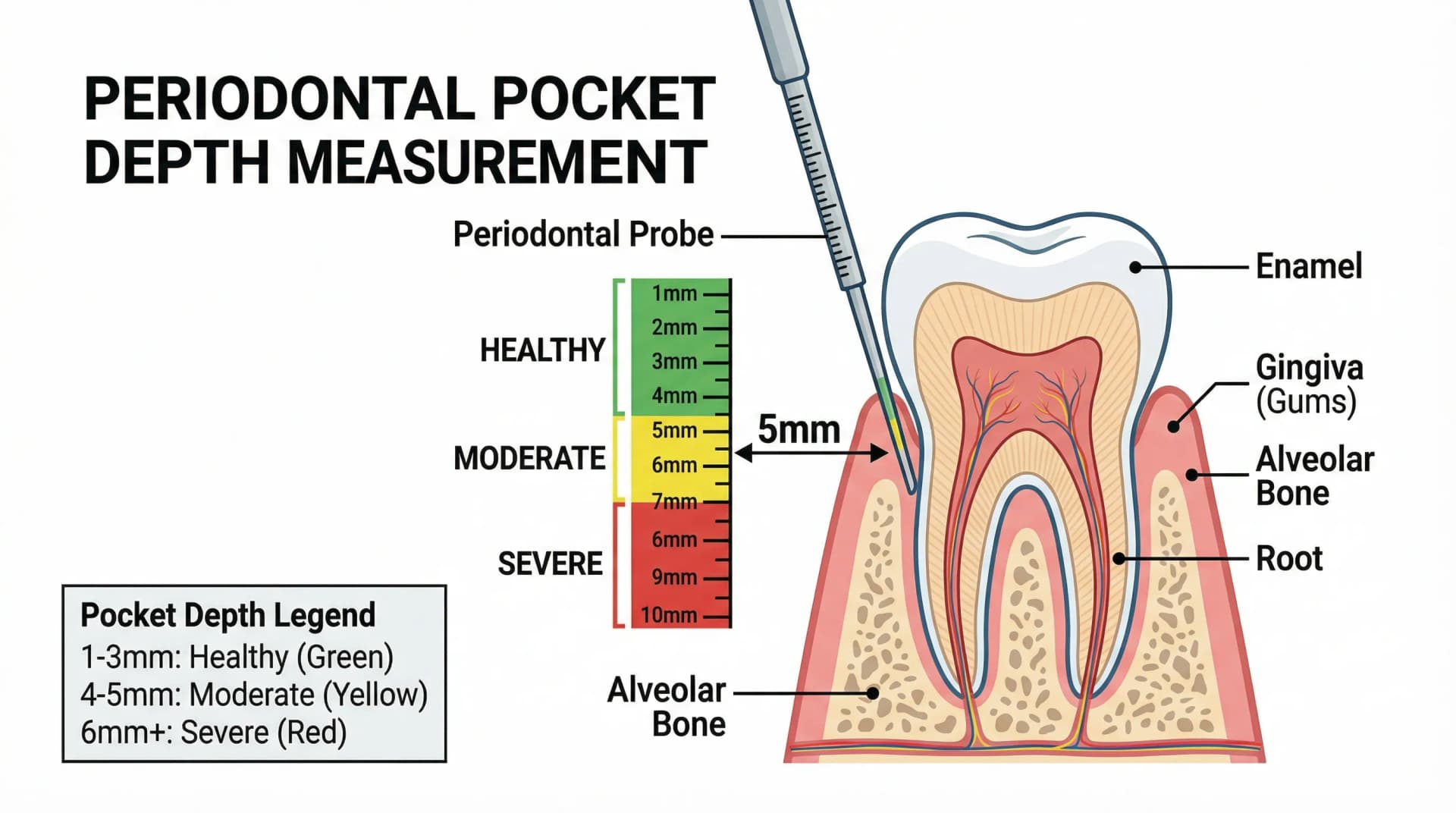
Periodontal pocket depth is one of the most important numbers your dentist measures. Healthy gums have pockets of 1-3mm. At 4mm, early periodontitis may be developing. At 5-6mm, moderate disease is likely present. And 7mm or deeper signals severe periodontitis that may threaten tooth survival. Understanding your numbers helps you take the right action at the right time.
If you've ever sat in a dental chair while someone called out a string of numbers — "3, 3, 2, 4, 3, 5" — you were hearing your periodontal pocket depth measurements. Those numbers may sound routine, but they tell a critical story about your gum health.
Let's break down exactly what those numbers mean, why they matter, and what you can do about them.
What Are Periodontal Pockets?
Every tooth sits inside a small groove where the gum tissue meets the tooth surface. This groove is called the gingival sulcus. In healthy gums, this space is shallow and tight, acting like a natural seal that keeps bacteria out.
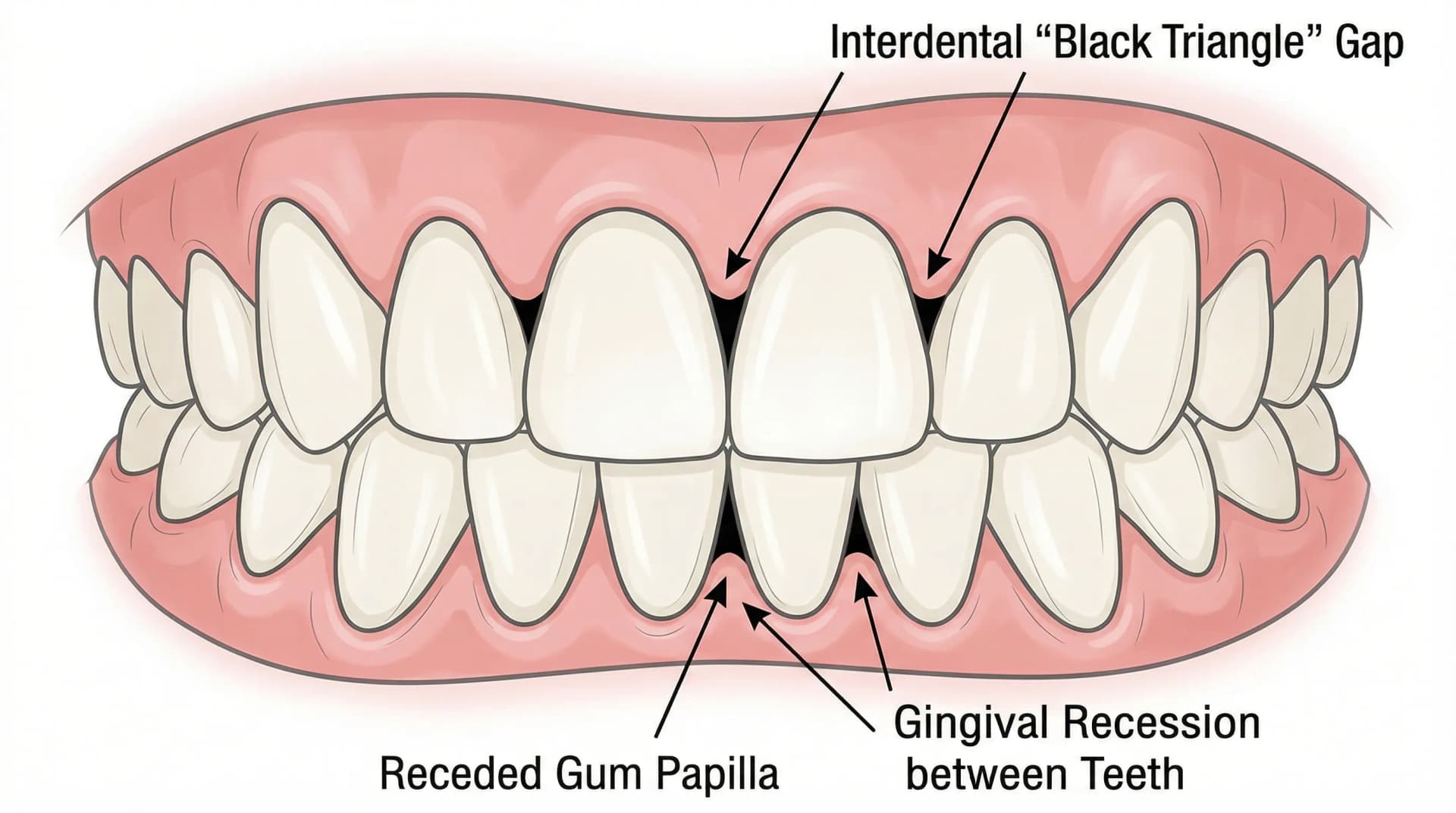
When gum disease develops, bacteria and plaque accumulate at the gumline, triggering an inflammatory response. Over time, this inflammation destroys the connective tissue and bone that hold the gum snug against the tooth. The sulcus deepens into what dentists call a periodontal pocket.
The deeper the pocket, the more tissue and bone have been lost — and the harder it becomes for you (or even your dentist) to clean the area effectively.
How Pocket Depth Is Measured
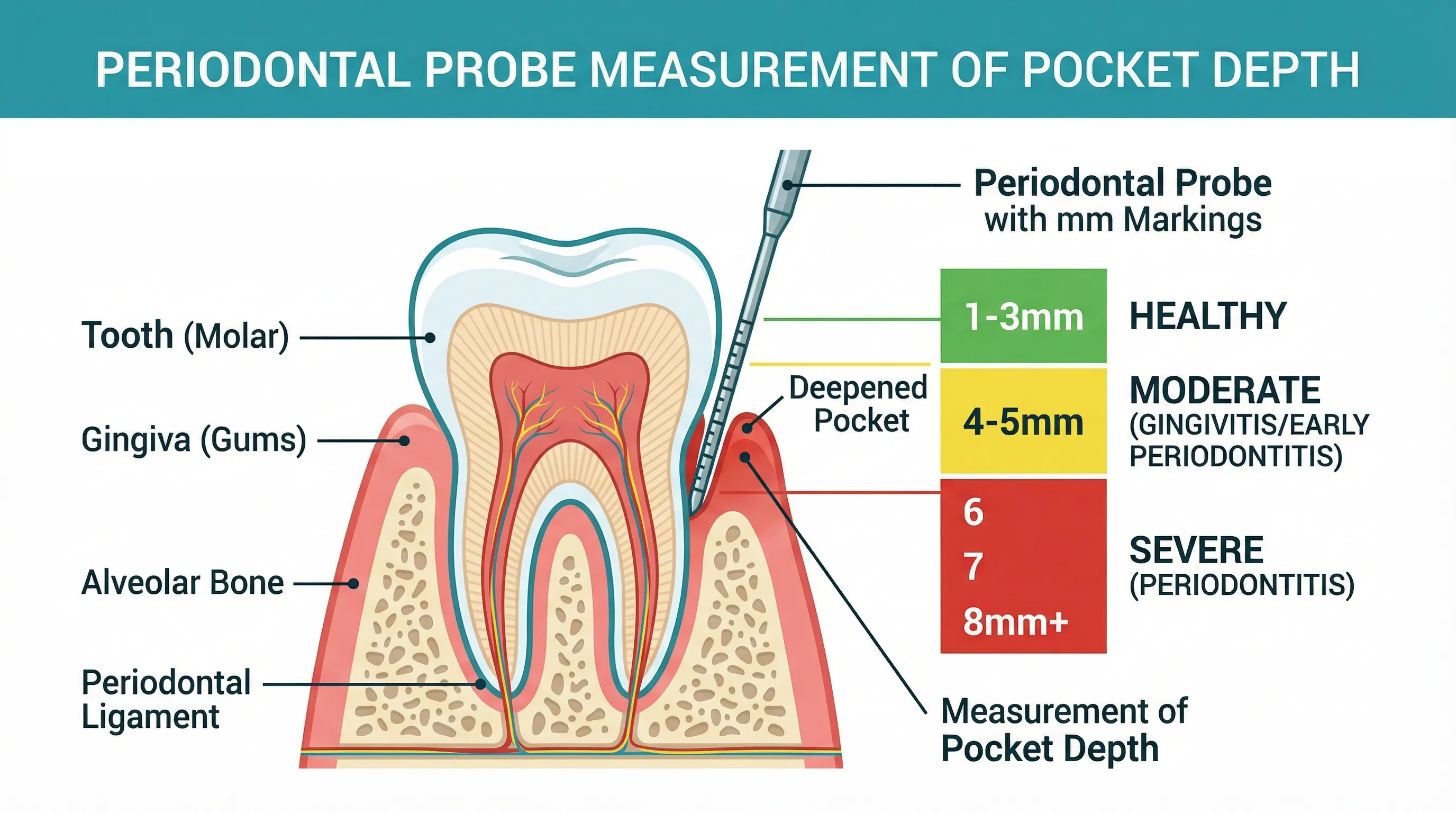
Your dentist or dental hygienist measures pocket depth using a periodontal probe — a thin, calibrated instrument marked in millimeter increments. The probe is gently inserted into the space between the gum and the tooth at six points around each tooth: three on the cheek side and three on the tongue side.
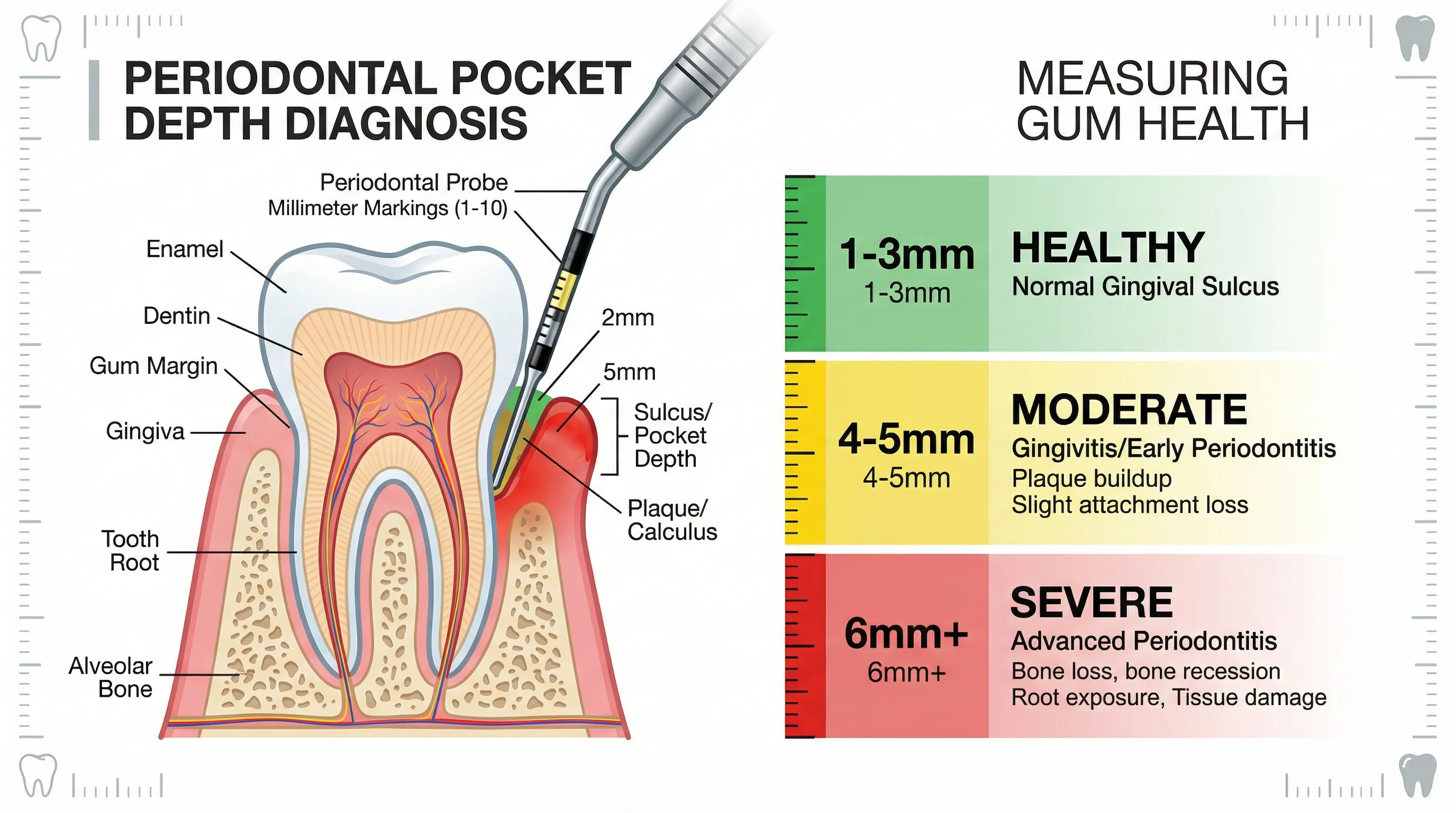
The measurement records how deep the probe can travel before it meets resistance. Healthy tissue resists the probe at a shallow depth. Diseased tissue lets the probe sink deeper because the attachment has broken down.
This process is called a full periodontal charting and is recommended at least once a year by the American Academy of Periodontology. A study in the Journal of Dental Research (2012) confirmed that regular periodontal probing is the most reliable clinical method for detecting periodontitis progression.
The process shouldn't be painful if your gums are healthy. If you feel significant discomfort during probing, that itself may be a sign of inflamed tissue.
The Gum Pocket Depth Chart: What Each Range Means
1-3mm: Healthy
This is the normal range. A depth of 1-3mm with no bleeding on probing indicates healthy gum tissue with intact attachment.
What it means:
- Gum tissue is firm and pink (or naturally pigmented)
- The attachment between tooth and gum is intact
- No bone loss is present
- Your home care is working
What to do: Maintain your current routine — brush twice daily with proper technique, floss daily, and keep up with regular dental cleanings every six months. You're in good shape.
4mm: Early Warning / Early Periodontitis
A 4mm reading is the clinical threshold that gets your dentist's attention. It may indicate the beginning of attachment loss, though not always — some areas naturally measure 4mm, especially around back teeth.
What it means:
- The gum attachment may be starting to break down
- Bacteria can accumulate in a 4mm pocket that a toothbrush can't fully reach
- Bleeding on probing at this depth is a stronger indicator of active disease than the number alone
- Radiographic (X-ray) evidence of bone loss may or may not be present
A landmark study in the Journal of Clinical Periodontology (2018) established that 4mm pockets with bleeding on probing represent the most reliable threshold for identifying sites at risk of further breakdown.
What to do: This is the stage where intervention makes the biggest difference. Your dentist may recommend more frequent cleanings (every 3-4 months instead of 6), improved home care techniques, and possibly localized scaling. If caught here, progression can often be halted.
5-6mm: Moderate Periodontitis
Pockets of 5-6mm indicate that significant attachment loss has occurred. Bone loss is typically visible on X-rays at this stage.
What it means:
- Connective tissue and bone supporting the tooth have been destroyed
- These pockets harbor anaerobic bacteria (like Porphyromonas gingivalis and Treponema denticola) that thrive in deep, oxygen-poor environments — the same bacteria implicated in cavities and tooth decay
- The bacteria in 5-6mm pockets are impossible to reach with brushing or flossing alone
- Without treatment, these sites will almost certainly worsen
Research published in the Journal of Periodontology (2015) found that untreated 5-6mm pockets progressed to deeper measurements within 12-24 months in the majority of patients.
What to do: Professional treatment is necessary at this stage. Scaling and root planing (SRP) — sometimes called "deep cleaning" — is the standard first-line treatment. During SRP, your dentist or hygienist removes plaque and calculus from below the gumline and smooths the root surfaces so gum tissue can reattach.
After SRP, a study in the Journal of Clinical Periodontology (2002) found that 5mm pockets were reduced by an average of 1.3mm, and 6mm pockets by 1.7mm. Combined with consistent home care, many patients stabilize at manageable depths.
7mm and Deeper: Severe Periodontitis
Pockets of 7mm or more represent advanced periodontal disease. This level of attachment and bone loss poses a direct threat to tooth retention.
What it means:
- Substantial bone loss has occurred around the affected teeth
- Teeth may feel loose or have shifted position
- The bacterial biofilm at this depth is highly organized and resistant to disruption
- Risk of tooth loss is significant without aggressive treatment
What to do: Consult your dentist or, ideally, a periodontist (a gum disease specialist). Treatment may include surgical options such as flap surgery (where the gum is lifted back for direct access to the root surface and bone), bone grafting, or guided tissue regeneration. In some cases, teeth with 7mm+ pockets around multiple roots may not be salvageable.
The goal at this stage isn't reversal — it's stabilization and saving as many teeth as possible.
Why Bleeding on Probing Matters as Much as Depth
Pocket depth alone doesn't tell the whole story. Your dentist also records whether each site bleeds when probed. Bleeding on probing (BOP) indicates active inflammation — a sign that the disease is currently progressing at that site.
A 4mm pocket that doesn't bleed may be stable and not require immediate intervention. A 4mm pocket that bleeds is a site in trouble. Research in Clinical Oral Investigations (2019) demonstrated that sites with both increased pocket depth and BOP were 4-6 times more likely to experience further attachment loss compared to deep sites without bleeding.
This is why the combination of depth measurements and BOP gives the most accurate picture of your periodontal status.
How to Improve Your Pocket Depth Numbers
While deep pockets (5mm+) require professional treatment, there's strong evidence that patients can improve borderline measurements (4mm) and maintain treatment results through home care:
Upgrade Your Oral Hygiene
A study in the International Journal of Dental Hygiene (2019) found that patients who switched to a powered toothbrush and added interdental brushes reduced 4mm pockets to 3mm within 3 months at significantly higher rates than those using manual brushes alone. The Modified Bass brushing technique — angling soft bristles at 45 degrees into the gumline with gentle vibrating strokes — is specifically designed to clean the sulcus.
Consider Oral Probiotics
Emerging research suggests that oral probiotics may support periodontal health. A systematic review in the Journal of Clinical Periodontology (2020) found that Lactobacillus reuteri supplementation, used as an adjunct to scaling and root planing, led to additional pocket depth reduction and reduced bleeding compared to SRP alone.
The proposed mechanism: beneficial bacteria compete with periodontal pathogens for colonization sites in the gum pocket, and certain strains produce antimicrobial compounds that inhibit pathogenic bacteria.

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim delivers 3.5 billion CFU of oral probiotic strains including L. reuteri in a dissolving tablet format. Research suggests these strains may support gum health by promoting a balanced oral microbiome.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
Anti-Inflammatory Nutrition
Your diet directly influences gum inflammation. A randomized controlled trial published in the Journal of Clinical Periodontology (2018) found that an anti-inflammatory diet (rich in omega-3 fatty acids, vitamin C, vitamin D, and fiber, and low in processed sugars) reduced gingival bleeding by 40% within 4 weeks — without any changes to oral hygiene habits.
Focus on:
- Vitamin C — Essential for collagen synthesis in gum tissue (bell peppers, strawberries, kiwi). See our full guide on vitamins for teeth and gums.
- Omega-3 fatty acids — Reduce inflammatory markers (salmon, sardines, walnuts)
- Vitamin D — Deficiency is associated with increased periodontitis severity (Journal of Periodontal Research, 2020)
- Green tea — EGCG catechins inhibit P. gingivalis growth (Archives of Oral Biology, 2016)
Don't Skip Your Maintenance Visits
After periodontal treatment, your dentist will typically recommend periodontal maintenance cleanings every 3-4 months. A long-term study in the Journal of Clinical Periodontology (2004) found that patients who adhered to a 3-month maintenance schedule lost 0.5 teeth over 11 years on average, while those who skipped maintenance lost 2.2 teeth over the same period.
These visits include repeat probing — which is how you track whether your numbers are improving, stable, or worsening.
When to See a Periodontist
Your general dentist handles the vast majority of gum disease cases. But a referral to a periodontist — a dentist with 3 additional years of specialized training — is appropriate when:
- You have multiple sites measuring 5mm or deeper
- Pocket depths are not improving after scaling and root planing
- You have generalized bone loss visible on X-rays
- Teeth are mobile or shifting
- You need surgical intervention (flap surgery, bone grafts, implants)
- You have systemic conditions (like diabetes) that complicate periodontal management
Don't hesitate to ask for a referral. Periodontists see complex cases daily and have tools and techniques that general practices may not offer.
Tracking Your Numbers Over Time
Ask your dental office for a copy of your periodontal charting at each visit. Many practices use digital charting software that can print comparison reports showing how your pocket depths have changed over time.
Seeing the numbers improve — a 5 dropping to a 4, a 4 returning to a 3 — is one of the most motivating aspects of taking gum health seriously. And seeing a number increase is an early warning that lets you act before real damage occurs.

ProDentim
Oral Probiotic for Gum & Teeth Health
Supporting your oral microbiome between dental visits with targeted probiotics like ProDentim may help maintain the pocket depth improvements you and your dentist work hard to achieve.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
Your pocket depth numbers are not a life sentence. They're a snapshot — and with the right combination of professional treatment and daily home care, most people can stabilize or improve their readings over time.
Related reading: