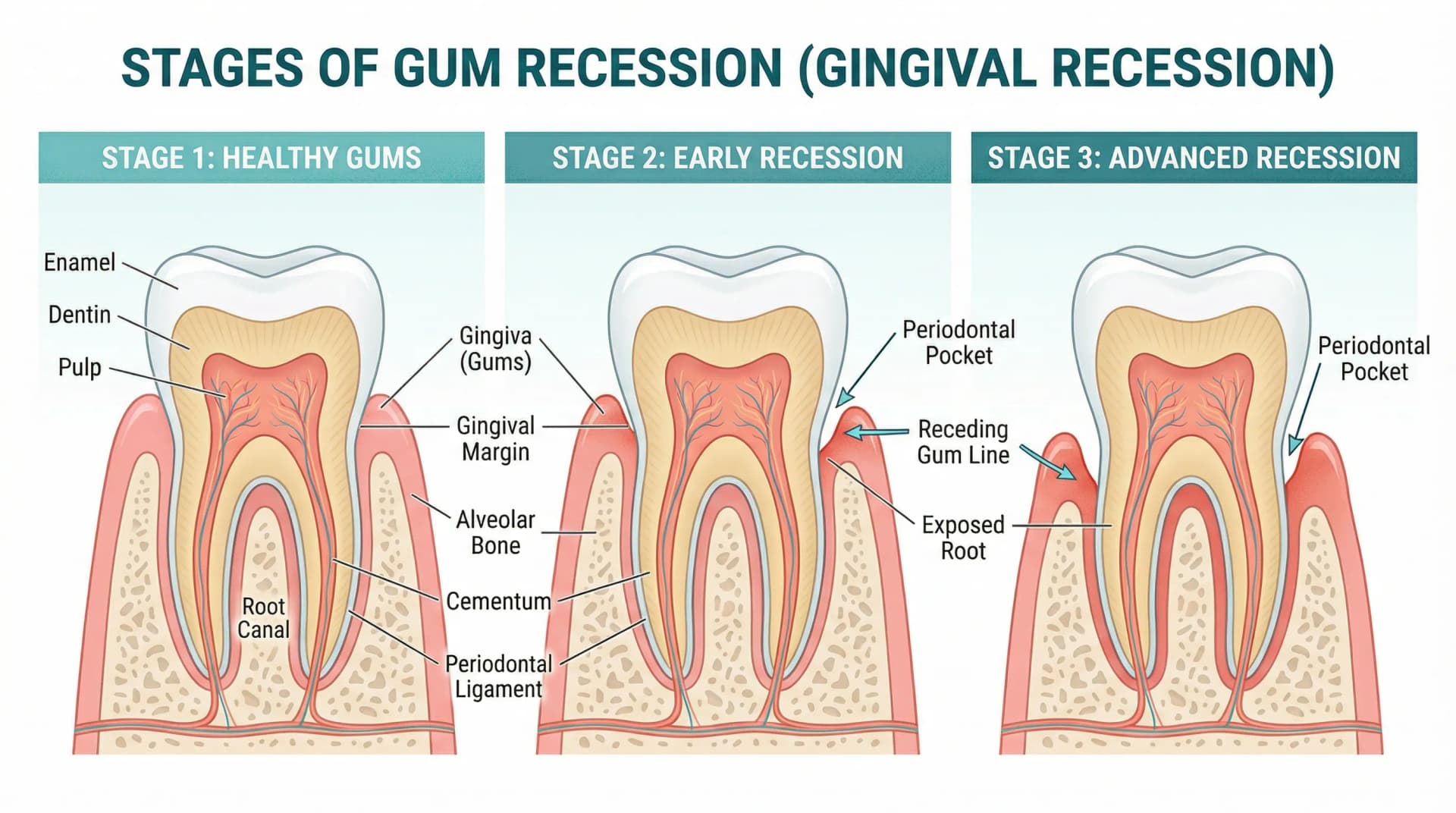
Tooth decay progresses through 5 distinct stages: (1) demineralization (white spots), (2) enamel decay, (3) dentin decay, (4) pulp involvement, and (5) abscess. The critical fact is that only Stage 1 is reversible — once a physical cavity has formed, professional treatment is required. Understanding these stages helps you recognize early warning signs and intervene before a reversible white spot becomes an irreversible cavity.
Tooth decay doesn't happen overnight. A cavity that requires a filling, root canal, or extraction today started as a microscopic change in the enamel weeks or months ago. At that earliest stage, it was completely reversible.
The problem is that most people don't know what the early stages look like, so they miss the window for prevention. By the time pain appears, the decay has usually progressed well beyond what home care can address.
Here's exactly what happens at each stage — and what can be done about it.
How Tooth Decay Starts
Before diving into the stages, it helps to understand the mechanism. Tooth decay is an infectious disease caused by specific bacteria — primarily Streptococcus mutans and Lactobacillus species. These bacteria form biofilms (plaque) on tooth surfaces and produce acid as they metabolize sugars from your diet.
The acid dissolves the mineral content of tooth enamel — a process called demineralization. When acid attacks occur faster than your body can repair the damage (remineralization), decay begins.
A study in Nature Reviews Disease Primers (2017) described dental caries as the result of a dysbiotic shift in the oral biofilm — essentially, an imbalance where acid-producing bacteria outnumber protective ones. Your diet plays a direct role in shaping this oral microbiome, and this understanding is important because it means decay is not inevitable; it results from a modifiable imbalance.
Stage 1: Demineralization (White Spot Lesions)
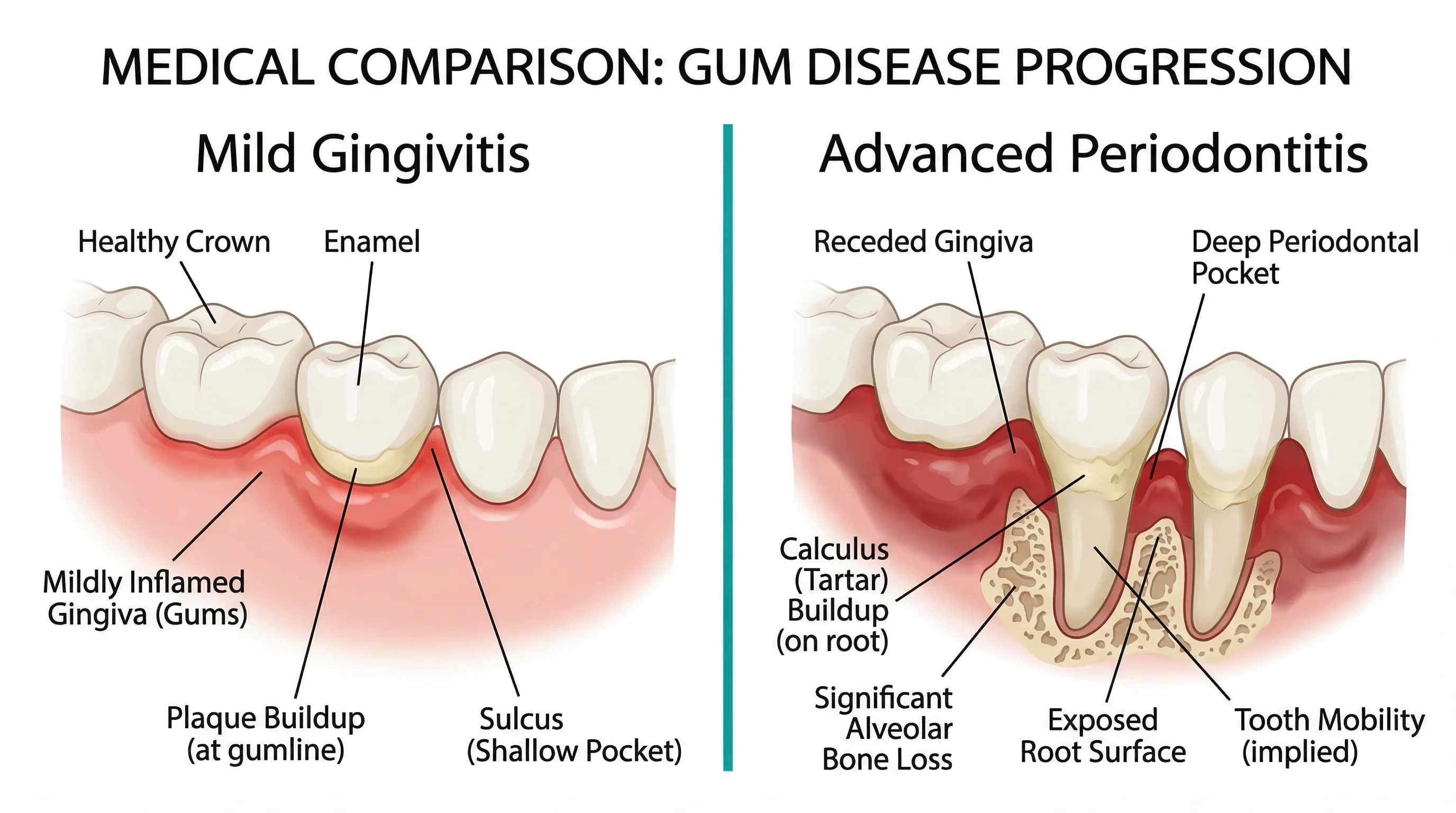
What's Happening
The first visible sign of tooth decay is a white spot lesion — a chalky, opaque white area on the tooth surface where minerals (calcium and phosphate) have been dissolved out of the enamel by bacterial acid.
At this stage, the enamel surface is still intact. There is no cavity, no hole, and no structural break. The enamel has lost mineral density but retains its physical structure. Think of it like a sponge that's had water squeezed out — the structure is there, but it's weakened and porous.
What It Looks Like
- Chalky white spots or patches on the tooth surface, especially near the gumline or between teeth
- The spots may be matte rather than glossy compared to healthy enamel
- Often visible on the front teeth, though they can appear anywhere
- No pain or sensitivity (the enamel layer has no nerve endings)
Can It Be Reversed?
Yes — this is the only stage where reversal is possible.
A systematic review in the Journal of Dental Research (2016) confirmed that white spot lesions can be remineralized through appropriate interventions. The lost minerals can be redeposited into the enamel crystal structure, restoring its density and strength.
Treatment
- Fluoride treatment — Professional fluoride varnish (22,600 ppm) applied by a dentist can accelerate remineralization. A Cochrane review (2013) found fluoride varnish reduced caries progression in primary teeth by 37%.
- Hydroxyapatite toothpaste — Supplies the native enamel mineral directly to the tooth surface. Research in the Journal of Dentistry (2019) showed comparable efficacy to fluoride for remineralization of early lesions.
- CPP-ACP (MI Paste) — Delivers bioavailable calcium and phosphate to the enamel. A study in the Journal of Dentistry (2018) found enhanced remineralization beyond fluoride alone.
- Dietary changes — Reduce sugar frequency, increase mineral-rich foods, and avoid acidic beverages between meals.
- Improved oral hygiene — Effective plaque removal reduces the bacterial acid load.

Denticore
Gum & Tooth Support Supplement
DentiCore provides calcium, phosphorus, and supporting nutrients that may help support the remineralization process during Stage 1 demineralization. Mineral supplementation works best alongside fluoride or hydroxyapatite toothpaste and dietary improvements.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
Timeline: With consistent intervention, visible improvement in white spot lesions typically takes 2-6 months. Patience is essential — remineralization is a gradual process.
Stage 2: Enamel Decay
What's Happening
If demineralization continues unchecked, the weakened enamel eventually breaks down physically. The surface layer collapses, creating a cavity — a structural hole in the enamel.
At this stage, the decay is still confined to the enamel layer (the outermost layer of the tooth, approximately 2.5mm thick on molar surfaces). The underlying dentin has not yet been reached.
Enamel has no nerves, which is why early cavities are typically painless. This is both good news (no discomfort yet) and dangerous (no warning signal that something is wrong).
What It Looks Like
- A visible hole, pit, or rough spot in the tooth surface
- Light brown or dark spots on the enamel
- Possible visible breakdown of the smooth enamel surface
- May be detectable on dental X-rays as a dark area within the enamel
- Still usually painless, though some sensitivity to sweet foods is possible
Can It Be Reversed?
No. Once the enamel surface has physically broken, remineralization cannot rebuild the lost structure. The cavity will not heal on its own. However, the decay can be stopped from progressing further with prompt treatment.
Treatment
- Dental filling — The standard treatment. The decayed enamel is removed and replaced with a filling material (composite resin, amalgam, glass ionomer, or ceramic). This is a straightforward procedure, typically done with local anesthesia.
- Dental sealant — For very early enamel cavities in certain locations (especially pit-and-fissure cavities on molars), a dentist may place a sealant over the cavity to seal out bacteria and arrest the decay. This is sometimes called "sealing in" a small cavity, and research in the Journal of Dental Research (2014) supports this approach for small, non-cavitated or minimally cavitated enamel lesions.
Why not to wait: An enamel-only cavity is a small, inexpensive fix. Waiting allows it to progress to dentin, where treatment becomes more extensive and costly.
Stage 3: Dentin Decay

What's Happening
Once decay penetrates through the enamel, it reaches the dentin — the layer beneath the enamel that makes up the bulk of the tooth structure. Dentin is softer than enamel (about 5 times less mineralized), yellower in color, and — critically — it contains tubules that connect to the tooth's nerve.
This is where decay accelerates. Because dentin is less mineralized and more porous, bacteria can spread through it much faster than through enamel. The decay front often widens significantly once it reaches dentin, creating a larger area of damage beneath what may look like a small enamel defect on the surface.
A study in Operative Dentistry (2010) found that dentin caries progresses approximately 2-3 times faster than enamel caries due to the lower mineral content and tubular structure of dentin.
What It Looks Like
- Visible dark brown or black discoloration on the tooth
- A hole that may be visibly deeper than the enamel surface
- Sensitivity to hot, cold, and sweet foods and beverages — the dental tubules transmit stimuli toward the nerve
- Possible mild-to-moderate toothache, especially when eating
- On X-ray: a dark area extending beyond the enamel into the dentin
Can It Be Reversed?
No. Dentin decay requires professional treatment to remove the infected tissue and restore the tooth.
Treatment
- Larger dental filling — The decayed dentin is removed and the tooth is restored with a filling. The cavity is typically larger than an enamel-only cavity, requiring more tooth structure to be removed.
- Inlay or onlay — For more extensive dentin decay, a lab-fabricated restoration (inlay or onlay) may be more durable than a direct filling.
- Crown — If significant tooth structure has been lost, a crown (cap) may be needed to protect the remaining tooth.
Consult your dentist promptly if you experience new sensitivity or visible discoloration. Dentin decay is a race against time — the sooner it's treated, the more tooth structure can be preserved.
Stage 4: Pulp Involvement (Pulpitis)
What's Happening
If dentin decay continues advancing, it eventually reaches the pulp — the innermost chamber of the tooth containing blood vessels, nerves, and connective tissue. The pulp is the "living" part of the tooth.
When bacteria and their toxins reach the pulp, the body responds with inflammation — pulpitis. Pulpitis comes in two forms:
- Reversible pulpitis — The pulp is inflamed but not yet infected. Symptoms include sharp sensitivity to cold that resolves quickly when the stimulus is removed. If the cause (usually a deep cavity) is treated promptly, the pulp can recover.
- Irreversible pulpitis — The pulp is infected and cannot recover. Symptoms include spontaneous, throbbing pain that may wake you at night, prolonged pain after hot or cold stimuli, and pain that radiates to the ear, jaw, or temple.
A study in the International Endodontic Journal (2019) noted that the transition from reversible to irreversible pulpitis can occur gradually or rapidly, and clinical symptoms alone cannot always reliably distinguish between the two — diagnostic testing by a dentist is needed.
What It Looks Like
- Significant tooth pain — often described as throbbing, intense, or waking from sleep
- Pain with hot foods/beverages (a classic sign of pulp involvement, as opposed to the cold sensitivity of dentin decay)
- Possible swelling of the gum near the affected tooth
- The tooth may appear darkened or grayish (indicating a dying nerve)
- Pain may worsen when lying down (increased blood pressure to the head)
Can It Be Reversed?
Reversible pulpitis — possibly, with prompt removal of the cause and restoration of the tooth.
Irreversible pulpitis — no. The pulp tissue must be removed.
Treatment
- Root canal therapy — The most common treatment for irreversible pulpitis. The infected pulp is removed, the root canals are cleaned, shaped, and disinfected, then filled with a biocompatible material (gutta-percha). The tooth is then restored with a crown. Despite its reputation, modern root canal treatment has a success rate exceeding 95% (Journal of Endodontics, 2016) and is performed under local anesthesia with minimal discomfort.
- Pulp capping — For reversible pulpitis where the pulp exposure is very small and recent, a dentist may place a biocompatible material (calcium hydroxide or MTA) directly over the exposed pulp to encourage healing. Success rates are variable and depend on the extent of bacterial contamination.
Why not to wait: Untreated irreversible pulpitis will progress to Stage 5 (abscess), which involves infection spreading beyond the tooth into surrounding bone and soft tissue.
Stage 5: Abscess Formation
What's Happening
When the pulp dies from infection (necrosis), bacteria continue to multiply inside the tooth and eventually spread beyond the root tip into the surrounding jawbone and soft tissue. This creates a dental abscess — a pocket of pus formed by the body's immune response to the bacterial infection.
There are two main types:
- Periapical abscess — Forms at the tip of the tooth root. The most common type from progressive decay.
- Periodontal abscess — Forms in the gum tissue adjacent to the tooth root. More commonly associated with gum disease than tooth decay.
A dental abscess is a serious medical condition. The infection can spread to the jaw, neck, and in rare but life-threatening cases, the brain or bloodstream (sepsis). The British Dental Journal (2018) reported that dental infections still account for hospital admissions and, in rare cases, fatalities when left untreated.
What It Looks Like
- Severe, persistent, throbbing pain that may radiate to the jaw, ear, or neck
- Swelling in the face, cheek, or under the jaw
- A visible "gum boil" (parulis) — a pimple-like swelling on the gum near the affected tooth that may drain pus
- Fever, malaise, and feeling generally unwell
- Bad taste in the mouth (from draining pus)
- Difficulty opening the mouth or swallowing (if the infection has spread to soft tissue spaces)
- The tooth may be extremely sensitive to touch or pressure (even biting gently is painful)
Can It Be Reversed?
No. A dental abscess requires emergency professional treatment. It will not resolve on its own, and home remedies cannot eliminate the infection.
Treatment
- Incision and drainage — If a fluctuant (fluid-filled) abscess is present, the dentist may incise and drain it to provide immediate relief.
- Antibiotics — Prescribed when infection has spread beyond the tooth (facial swelling, fever, difficulty swallowing). Antibiotics alone cannot resolve a dental abscess — they control the spread while the source is treated. The most common first-line antibiotic is amoxicillin, with clindamycin as an alternative for penicillin-allergic patients. Be aware that antibiotics can disrupt your oral microbiome, so targeted use under professional guidance is important.
- Root canal therapy — If the tooth is salvageable, root canal treatment removes the source of infection and may allow the tooth to be preserved.
- Extraction — If the tooth cannot be saved (extensive destruction, fracture, or failed previous root canal), extraction removes the source of infection entirely.
Seek emergency care if: You have facial swelling that is spreading, difficulty breathing or swallowing, fever above 101°F (38.3°C), or the swelling is closing your eye. These signs indicate the infection is spreading to potentially dangerous tissue spaces and requires immediate hospital-based treatment.
Prevention: Stopping Decay Before It Starts
Understanding the stages makes prevention straightforward — the goal is to keep the demineralization/remineralization balance tilted in favor of remineralization:
Daily habits:
- Brush twice daily with fluoride or hydroxyapatite toothpaste (2 minutes each time)
- Floss once daily to clean between teeth where 40% of tooth surfaces are located
- Limit sugar and acid exposure to mealtimes (frequency matters more than total amount)
- Chew xylitol gum after meals to stimulate saliva and inhibit S. mutans
- Drink water throughout the day
Professional care:
- Dental checkups every 6 months (or as recommended by your dentist)
- Professional cleanings to remove tartar
- Dental sealants on permanent molars (especially for children and teenagers)
- Professional fluoride treatments for high-risk individuals
Nutritional support:
- Adequate calcium (1,000mg daily) and phosphorus for enamel strength
- Vitamin D3 (2,000-4,000 IU daily) for calcium absorption
- Vitamin K2 (100-200 mcg daily) for mineral deposition into teeth

Denticore
Gum & Tooth Support Supplement
DentiCore provides calcium, phosphorus, and supporting minerals for ongoing enamel and dentin support. Nutritional supplementation may help maintain the mineral supply your teeth need for the remineralization process, particularly during Stage 1 when reversal is still possible.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
The cost of prevention — a toothbrush, toothpaste, floss, and regular dental visits — is a fraction of the cost of treating advanced decay. A simple filling costs $150-300. A root canal with a crown costs $1,500-3,000. Prevention is not just healthier; it's dramatically more cost-effective.
Related reading: