Gum recession is caused by a combination of factors — most commonly aggressive brushing, periodontal disease, and genetics. Once gum tissue has receded, it cannot grow back naturally. However, understanding the causes allows you to stop further recession and protect your remaining gum tissue. The key is identifying which factors apply to you and addressing them before more tissue is lost.
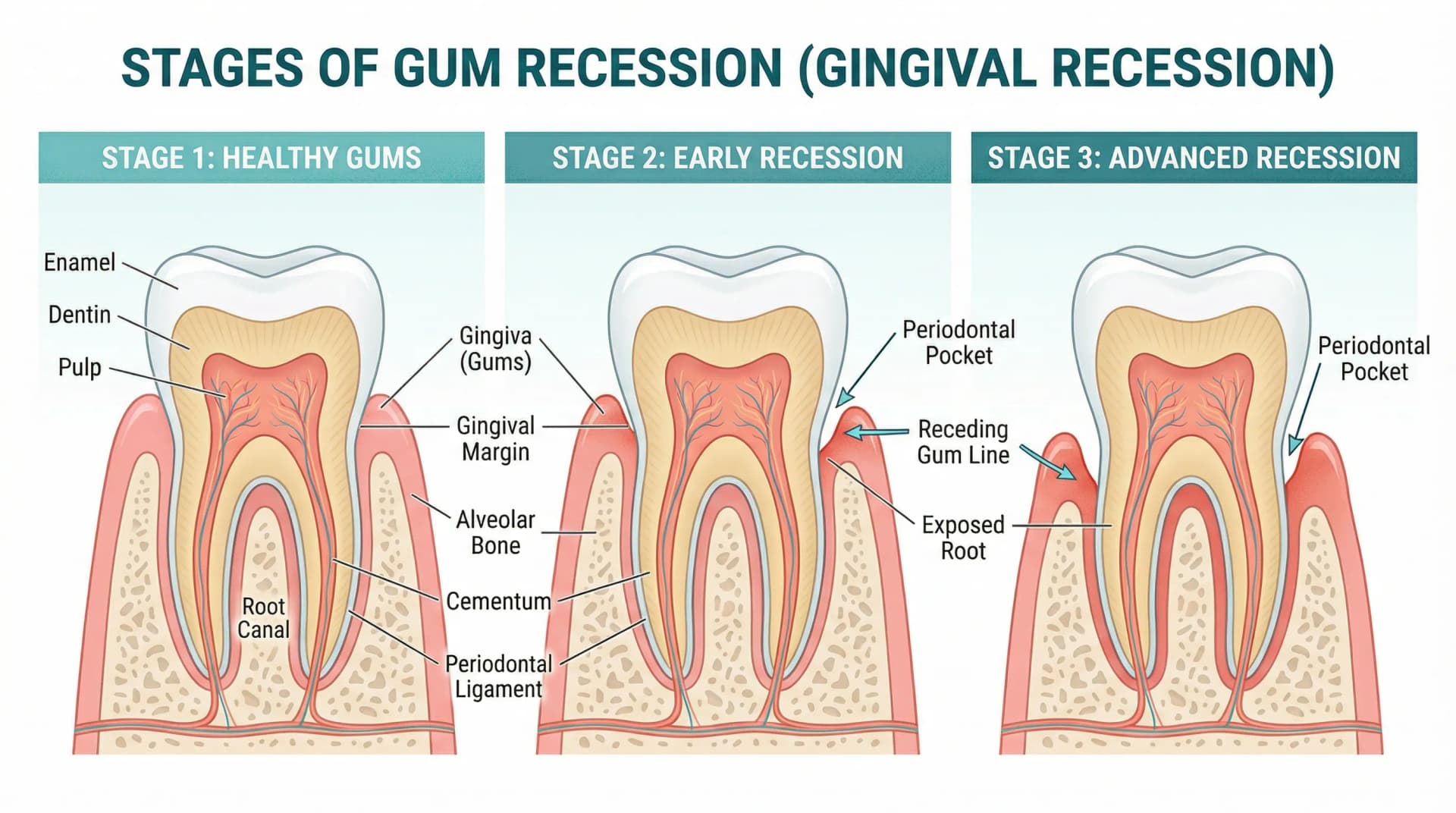
Gum recession — where the gum tissue pulls back from the tooth, exposing more of the tooth root — affects roughly 50% of adults over 30. It's gradual enough that many people don't notice it until significant tissue has been lost.
Here are the seven most common causes, ranked by how frequently they contribute to recession, along with what you can do about each one.
1. Aggressive Brushing (Toothbrush Abrasion)
How common: The #1 cause of non-disease-related recession
Many people brush their teeth like they're scrubbing a dirty pot — hard, fast, and with a heavy hand. This mechanical trauma physically damages the gum tissue over time.
How it causes recession:
- Hard-bristle brushes or excessive pressure abrade the delicate gum margin
- Horizontal, back-and-forth scrubbing motions are particularly destructive
- The outer (buccal/facial) surfaces of teeth are most affected because that's where brushing pressure is highest
- Over months and years, the gum tissue retreats from the chronic trauma
Warning signs:
- Bristles on your toothbrush splay out within a month of use
- Recession is worse on the canines and premolars (commonly the sites of highest brushing pressure)
- Sensitivity to cold on exposed root surfaces
- Notched grooves (abfraction lesions) appear at the gumline
- Recession pattern is on the outside surfaces of teeth, not between them
How to stop it:
- Switch to a soft-bristle brush immediately
- Use gentle circular motions (Modified Bass technique) instead of horizontal scrubbing
- Hold the brush with a light grip — think pencil grip, not hammer grip
- Consider an electric toothbrush with a pressure sensor that alerts you when you press too hard
- Set a 2-minute timer — people who rush tend to compensate by pressing harder
A study in the Journal of Clinical Periodontology (2003) found that reducing brushing force to under 150 grams prevented further recession, while forces above 300 grams accelerated it. Most electric toothbrushes with pressure sensors are calibrated to this threshold.
2. Periodontal Disease (Gum Disease)
How common: The #1 cause of disease-related recession
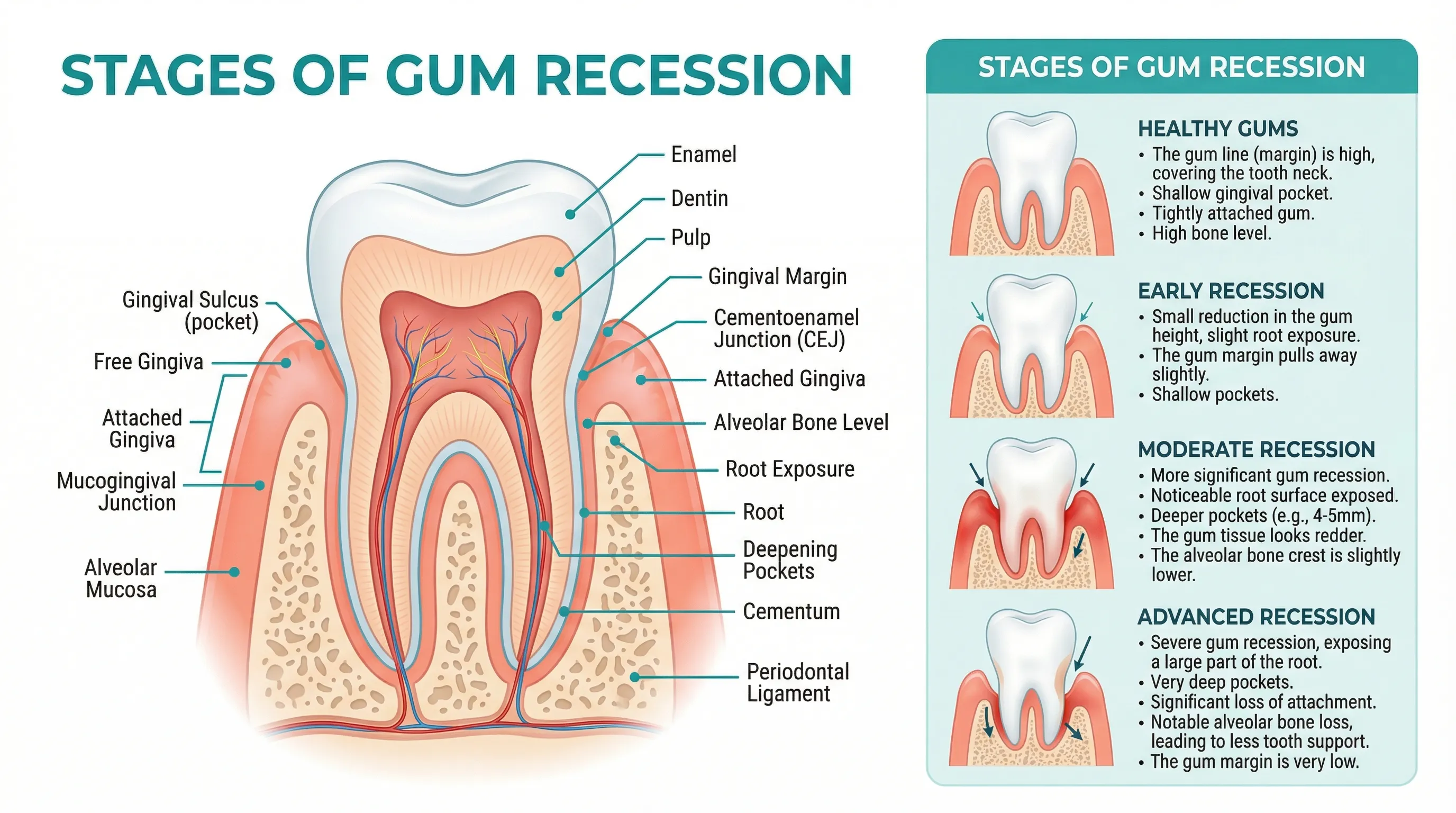
Chronic periodontitis destroys the bone and connective tissue that support teeth. As these structures deteriorate, the gum tissue that overlies them recedes.
How it causes recession:
- Bacterial toxins trigger chronic inflammation in gum tissue
- The inflammatory response destroys collagen fibers that attach gum to tooth
- Alveolar bone resorption removes the scaffold that gum tissue sits on
- As bone recedes, gum tissue follows — it can't remain where there's no underlying support
Warning signs:
- Bleeding gums (especially when brushing or flossing)
- Red, swollen, or tender gum tissue
- Bad breath that doesn't resolve with brushing
- Pockets deeper than 3mm on probing
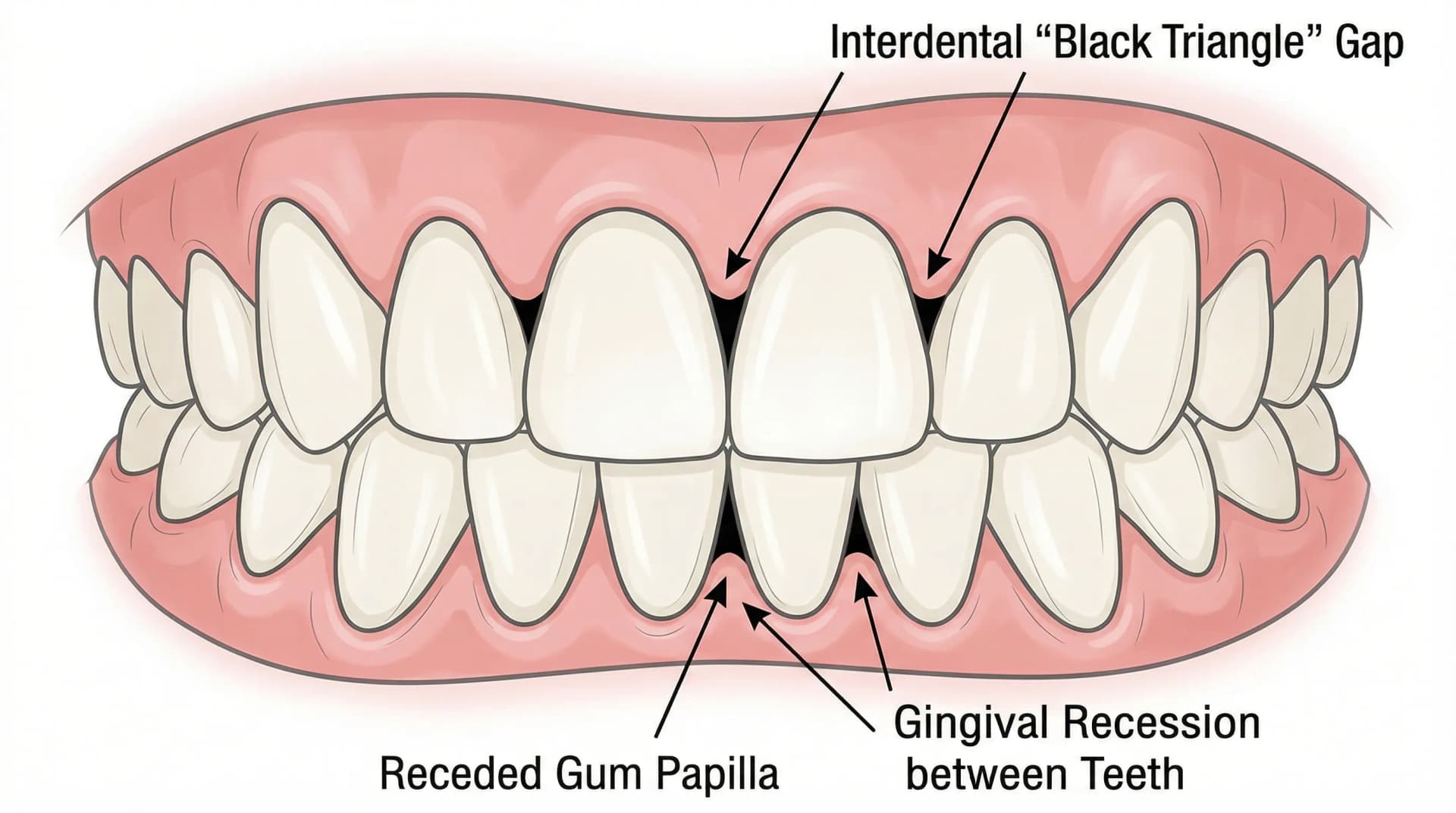
- Recession between teeth (interdental), not just on outer surfaces
How to stop it:
- See your dentist for periodontal assessment
- If pockets are 4mm+, scaling and root planing is needed
- Maintain excellent daily hygiene to prevent progression
- Quit smoking (the strongest modifiable risk factor for periodontal disease)
- Consider oral probiotics to support oral microbiome balance

ProDentim
Oral Probiotic for Gum & Teeth Health
For recession driven by periodontal disease, ProDentim's L. reuteri strain has clinical evidence for reducing the inflammation and pathogenic bacteria that destroy gum tissue attachment.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
3. Genetics
How common: A factor in approximately 30% of gum disease cases
Some people are simply more genetically susceptible to gum recession, regardless of how well they care for their teeth.
How genetics contribute:
- Thin gum tissue biotype — People with naturally thin, delicate gums are more vulnerable to recession than those with thick, fibrous tissue. This is an inherited trait.
- Immune response variations — Genetic polymorphisms in IL-1 (interleukin-1) genes affect how aggressively your immune system responds to plaque bacteria. Overactive immune responses cause more collateral tissue damage.
- Tooth position/alignment — Genetically determined jaw size and tooth alignment affect how forces distribute across the gumline.
A twin study published in the Journal of Dental Research (2017) found that genetic factors accounted for approximately 38% of the variance in clinical attachment loss — a key measure of gum recession.
How to manage it:
- You can't change your genetics, but you can be more vigilant about prevention
- If you have thin gum tissue, be especially careful with brushing pressure
- More frequent dental check-ups (every 4-6 months instead of every 6-12)
- Consider preventive gum grafting if a dentist identifies high-risk areas
4. Bruxism (Teeth Grinding and Clenching)
How common: Affects 8-31% of adults
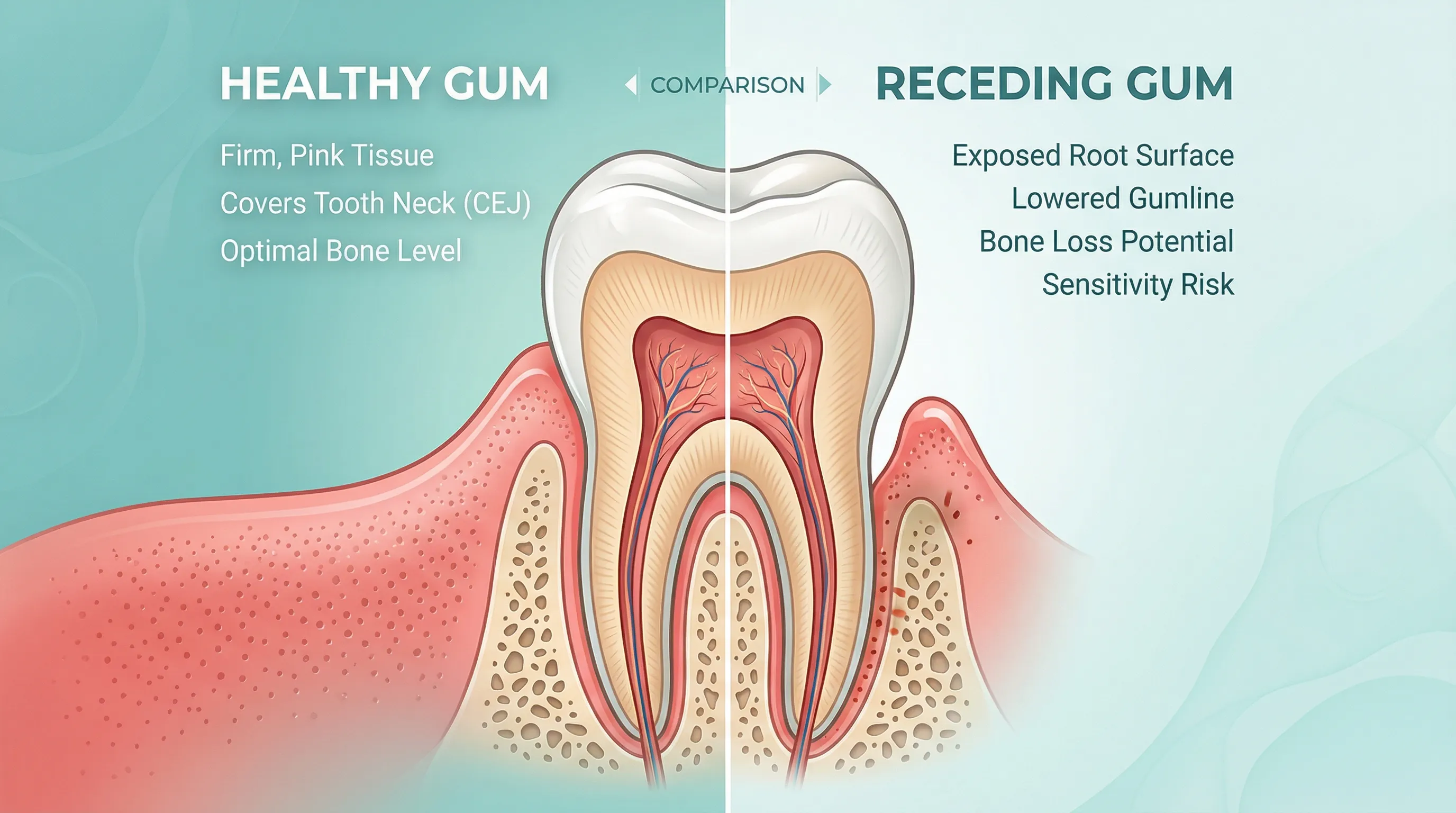
Bruxism places enormous lateral and compressive forces on teeth — forces they weren't designed to handle. Over time, these forces can cause or accelerate gum recession.
How it causes recession:
- Excessive force flexes the tooth at the gumline, creating micro-fractures in enamel (abfraction lesions)
- The chronic stress on the periodontal ligament causes bone remodeling and loss
- Gum tissue cannot maintain attachment to a tooth that's constantly being rocked by grinding forces
- Night grinding is particularly destructive because forces are up to 6x stronger than normal chewing
Warning signs:
- Notched, V-shaped grooves at the gumline of teeth (abfraction)
- Flat, worn tooth surfaces (especially molars)
- Morning jaw pain, headaches, or facial soreness
- Cracked or chipped teeth
- Partner reports hearing grinding sounds at night
How to stop it:
- Get a custom night guard from your dentist (over-the-counter guards are less effective and can worsen the problem)
- Address underlying causes: stress management, sleep apnea treatment
- Avoid caffeine and alcohol before bed (both increase grinding)
- Consider Botox injections for severe bruxism (reduces masseter muscle force)
5. Tobacco Use
How common: 42% of periodontitis cases in the US are attributable to smoking
Tobacco use is the strongest modifiable risk factor for gum disease and recession.
How it causes recession:
- Reduced blood flow — Nicotine constricts blood vessels in gum tissue, reducing oxygen and nutrient delivery. This impairs healing and makes tissue more vulnerable to breakdown.
- Impaired immune response — Smoking compromises neutrophil function, reducing the body's ability to fight periodontal bacteria
- Altered oral microbiome — Smokers harbor more pathogenic bacteria and fewer beneficial species. Antibiotics can cause similar disruptions to oral bacterial balance.
- Masked symptoms — Vasoconstriction reduces bleeding, so smokers often don't notice gum disease until it's advanced
The numbers: Smokers are 2-6x more likely to develop periodontitis than non-smokers. A meta-analysis in the Journal of Periodontology (2018) found that smoking was the single strongest risk factor for progressive periodontal attachment loss.
How to stop it:
- Quit smoking. There is no safe level of tobacco use for gum health.
- After quitting, gum health improves within weeks, and periodontitis risk approaches non-smoker levels within 10 years
- Smokeless tobacco (chewing tobacco, snuff) is equally harmful to gums and also causes recession at the specific contact site
6. Hormonal Changes
How common: Affects the majority of women during pregnancy, puberty, and menopause
Hormonal fluctuations — particularly in estrogen and progesterone — directly affect gum tissue sensitivity and blood flow.
How hormones contribute:
- Pregnancy: Elevated progesterone increases blood flow to gums and amplifies the inflammatory response to plaque. Pregnancy gingivitis affects 60-75% of pregnant women and can accelerate recession if not managed.
- Menopause: Declining estrogen thins gum tissue, reduces collagen density, and may decrease saliva production — all of which increase recession vulnerability.
- Hormonal contraceptives: Older high-dose formulations were linked to gingival inflammation; modern low-dose pills have a smaller effect.
- Puberty: Hormonal surges increase gingival sensitivity, but recession at this age is rare.
How to manage it:
- Maintain impeccable oral hygiene during hormonal transitions
- See your dentist for a cleaning during the second trimester of pregnancy
- Post-menopausal women should discuss gum health with both dentist and gynecologist
- Consider HRT's potential gum health benefits if appropriate for your overall health situation
7. Tooth Misalignment and Orthodontic Issues
How common: Varies, but a factor in many localized recession cases
When teeth are misaligned — crowded, rotated, or positioned outside the normal arch — the bone and gum tissue may not adequately cover the root surface.
How it causes recession:
- Teeth outside the bony arch (labially positioned) have thinner bone coverage, making overlying gum tissue vulnerable
- Crowded teeth make plaque removal difficult, increasing gum disease risk
- Orthodontic treatment itself can cause recession if teeth are moved too quickly or too far outside the bone
- Lip and tongue piercings can cause localized recession from repeated tissue trauma
How to stop it:
- Orthodontic correction can improve long-term gum health by aligning teeth within the bony arch
- However, discuss recession risk with your orthodontist before treatment
- Slow, controlled tooth movement with monitoring is key
- Remove oral piercings that contact gum tissue
Prevention: 8 Steps to Protect Your Gums
- Use a soft-bristle brush with gentle pressure
- Floss daily to prevent plaque-driven recession between teeth
- Don't smoke — it's the most impactful change you can make
- Get a night guard if you grind your teeth
- See your dentist every 6 months (or more frequently if you have risk factors)
- Eat a nutrient-rich diet — vitamin C, D, K, and omega-3s support gum tissue
- Consider oral probiotics — L. reuteri has evidence for reducing the inflammation that drives recession. See our ProDentim review for one well-formulated option.
- Address misalignment — talk to an orthodontist about crowded or malpositioned teeth
When to See a Specialist
See a periodontist (gum specialist) if:
- Recession is progressing despite good hygiene
- Root surfaces are exposed and sensitive
- Aesthetics are a concern (recession visible when you smile)
- Your dentist measures pockets deeper than 4mm
Treatment options for established recession include gum graft surgery, the pinhole surgical technique (PST), guided tissue regeneration, and enamel matrix derivatives. These procedures can cover exposed roots and protect against further loss.
Related reading: