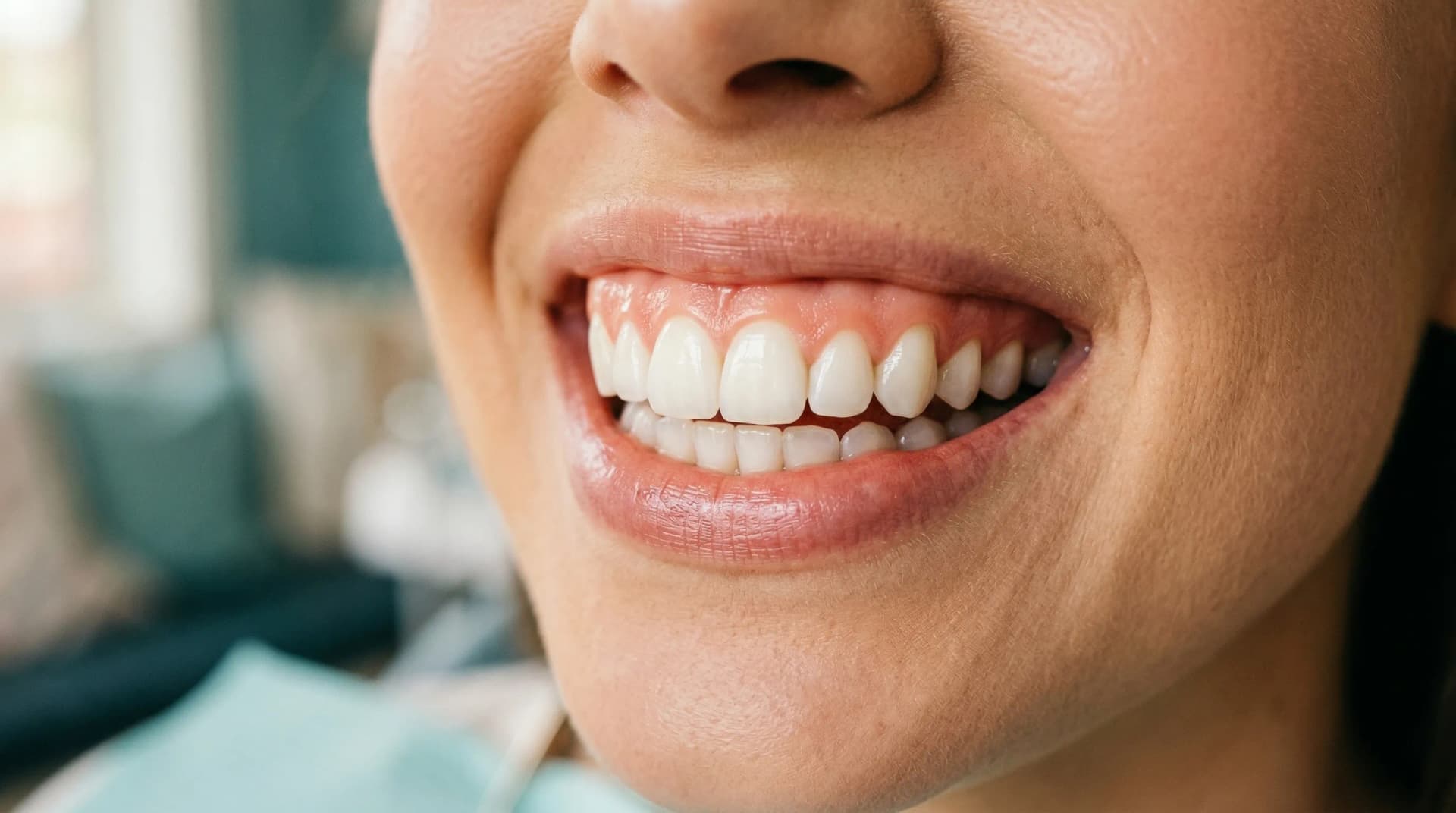
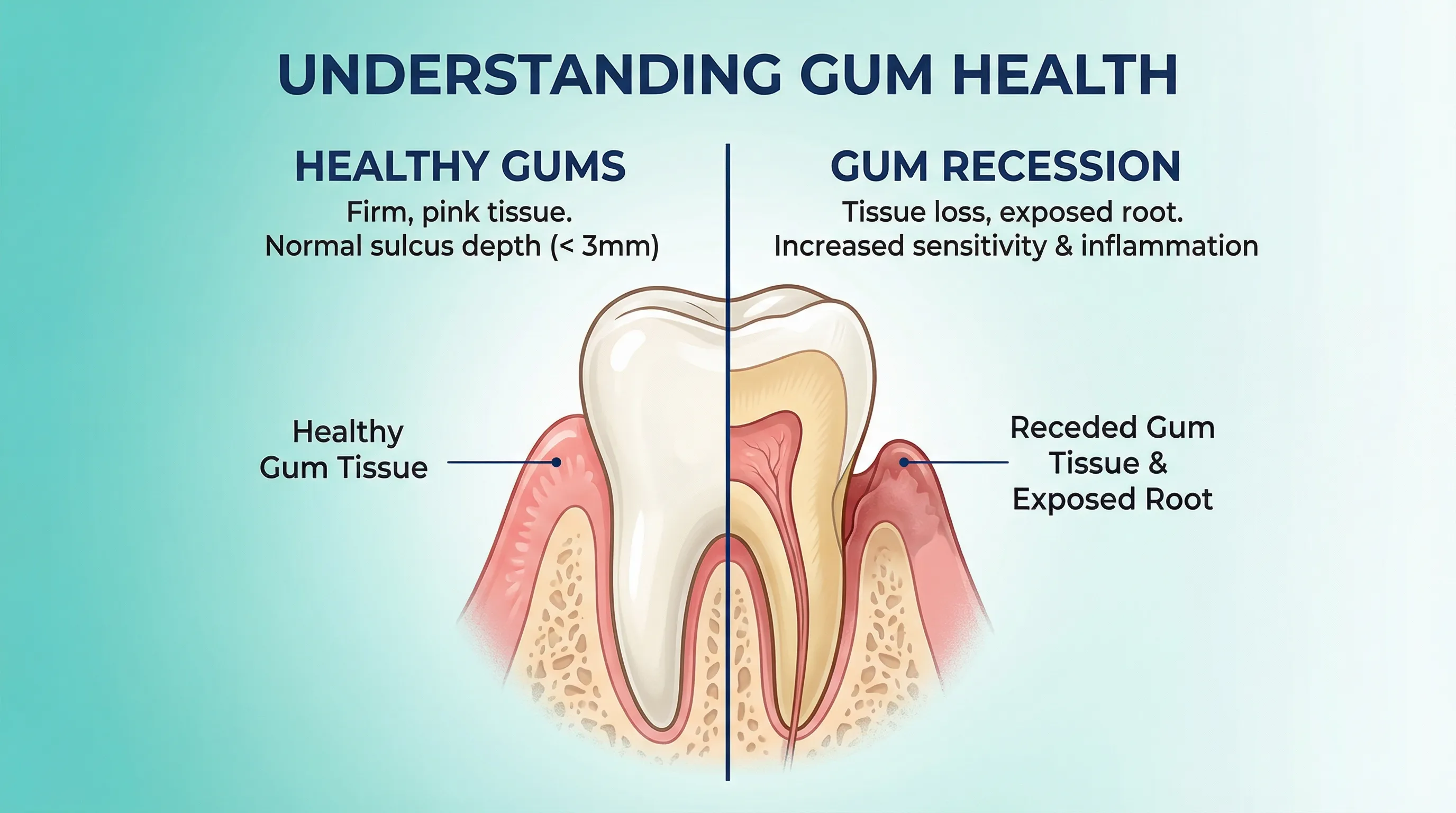
Healthy gums are typically coral pink (though natural variation exists across skin tones), firm to the touch, stippled in texture like an orange peel, and do not bleed when you brush or floss. Learning to recognize these visual markers helps you spot early signs of gum disease before they progress into something more serious.
Most people have a pretty good sense of what a healthy smile looks like in terms of teeth — white, straight, no visible cavities. But when it comes to gums, many of us have never really thought about what "healthy" is supposed to look like. That's a problem, because your gums are the foundation everything else sits on. If the foundation is compromised, even the best-looking teeth are at risk.
This guide will walk you through exactly what to look for when you examine your own gums, what's normal, what's not, and how to perform a simple self-check at home.
Why Your Gums Matter More Than You Think
Gum tissue (gingiva) doesn't just fill the space between your teeth for aesthetic reasons. It forms a protective seal around each tooth, acting as a barrier against the billions of bacteria living in your mouth. When that seal breaks down — through inflammation, recession, or disease — bacteria gain access to the bone and ligaments that hold your teeth in place.
The Centers for Disease Control and Prevention (CDC) estimates that nearly half of American adults aged 30 and older have some form of periodontal disease. The earliest stages are often painless and visually subtle, which is why knowing what healthy gums look like is your first line of defense.
The Five Signs of Healthy Gums
1. Color: Coral Pink (With Natural Variation)
Healthy gum tissue in people with lighter skin tones is typically described as "coral pink" or "salmon pink." This color indicates good blood circulation and an absence of significant inflammation.
However — and this is an important point that many dental resources overlook — gum color varies naturally with skin tone and ethnicity. People with darker complexions often have gums that range from brownish-pink to dark brown, and this is completely normal. This natural pigmentation is caused by melanin, the same pigment responsible for skin color.
A 2003 study in the Journal of Periodontology documented the wide range of normal gum pigmentation across different ethnic groups and confirmed that melanin pigmentation is a physiological (not pathological) finding.
What to watch for: The key is not a specific shade but rather changes from your personal baseline. If your normally pink gums turn red, or if your naturally brown gums develop areas that look darker, redder, or purplish, that's worth investigating.
2. Texture: Stippled Like an Orange Peel
Run your tongue along your gums, or look closely in a mirror. Healthy attached gingiva has a slightly bumpy, dimpled surface that's often compared to the skin of an orange. This texture is called stippling, and it's created by the connective tissue fibers that attach the gum tissue firmly to the underlying bone.
According to Carranza's Clinical Periodontology — one of the definitive textbooks in the field — stippling is present in about 40% of adults and is considered a sign of healthy, well-keratinized gum tissue. However, the absence of visible stippling doesn't necessarily indicate disease, as it varies from person to person.
When gums become inflamed (as in gingivitis), the tissue swells and stippling may disappear. The gums take on a smooth, shiny, or "glossy" appearance instead. This loss of stippling is one of the earliest visual clues that something is changing.
3. Shape: Knife-Edge Margins and Pointed Papillae
The anatomy of healthy gums has specific landmarks that dentists and hygienists assess at every checkup:
- Gingival margin — the edge where the gum meets the tooth. In health, this margin is thin and tapered, sometimes described as "knife-edge." It fits snugly against the tooth like a turtleneck fits around your neck.
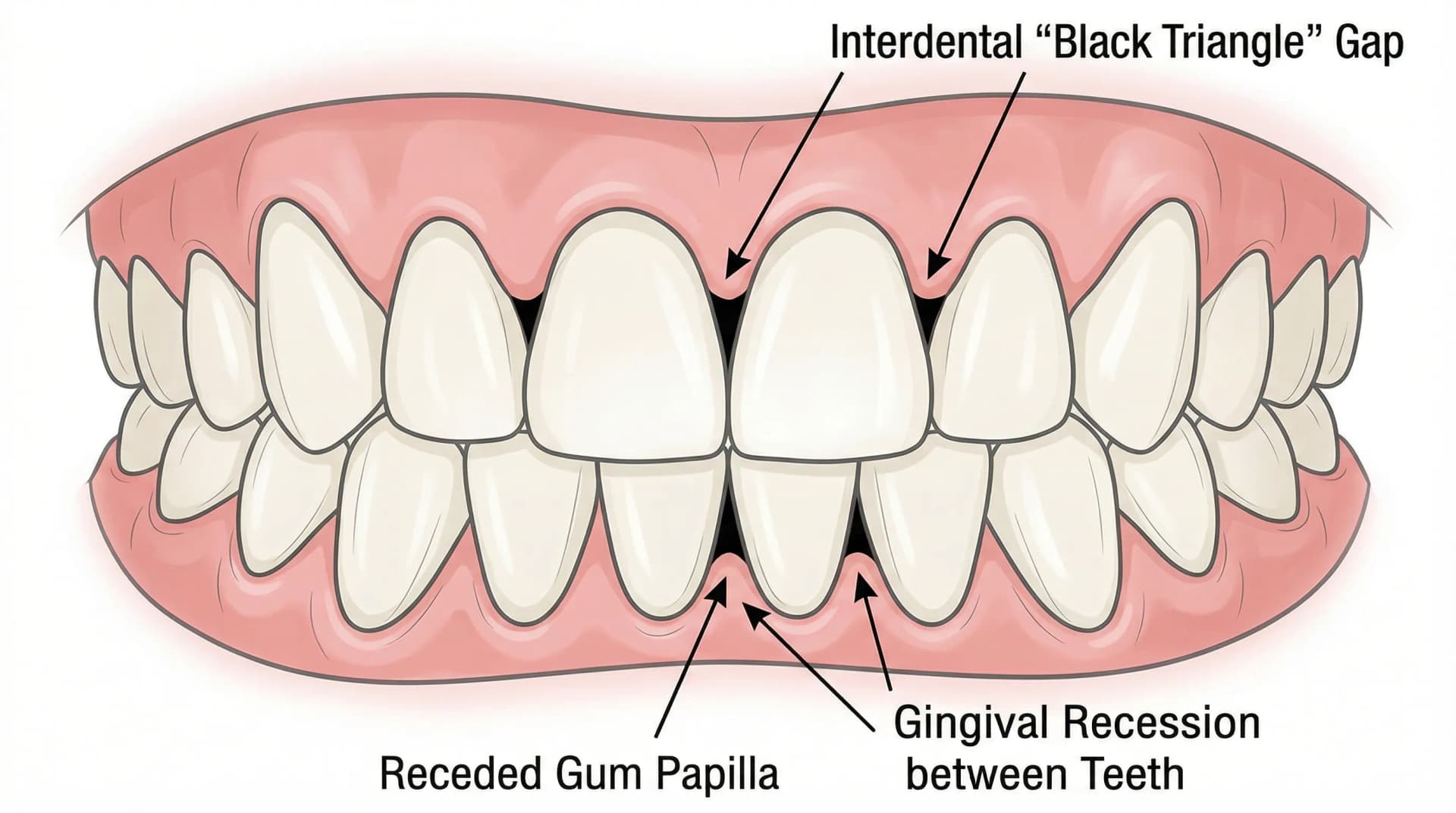
- Interdental papillae — the small, triangular points of gum tissue that fill the spaces between your teeth. In healthy gums, these papillae come to a point and completely fill the embrasure (the space between teeth). There should be no visible gaps or "black triangles."
- Free gingiva — the unattached portion of gum that forms a shallow groove (sulcus) around each tooth. In health, this sulcus is typically 1 to 3 millimeters deep.
When gums are swollen, the margins become thick and rounded (sometimes called "rolled margins"), and the papillae may appear bulbous rather than pointed.
4. Firmness: Resilient and Tightly Adapted
Healthy gums feel firm when you press on them gently — not spongy, puffy, or tender. They're tightly adapted to the tooth surface and don't pull away when you use an interdental brush or floss.
This firmness comes from the dense network of collagen fibers within the gum tissue. A 2012 review in the Journal of Oral Biology and Craniofacial Research described how the structural integrity of gingival collagen is essential for maintaining periodontal health, and how inflammatory processes break down these fibers, leading to the soft, swollen tissue characteristic of gum disease.
If you press on your gums with a clean finger and they feel mushy or leave an indentation, that may suggest edema (fluid retention from inflammation).
5. No Bleeding on Brushing or Flossing
This is perhaps the most important sign of all — and the one most people get wrong. Healthy gums do not bleed. Not when you brush. Not when you floss. Not even during a dental cleaning (or at most, very minimally).
If your gums bleed when you brush or floss, that's inflammation. The bleeding occurs because inflamed gum tissue develops new, fragile blood vessels (a process called angiogenesis) as part of the body's inflammatory response to bacterial plaque.
A landmark study by Loe, Theilade, and Jensen published in the Journal of Periodontology (1965) — the classic "experimental gingivitis" study — demonstrated that when plaque was allowed to accumulate for just 10 to 21 days, every participant developed gingivitis with bleeding on probing. When oral hygiene was resumed, the inflammation resolved completely.
The takeaway: bleeding gums are not normal, and they are almost always reversible with improved oral hygiene.
What Unhealthy Gums Look Like: Warning Signs
Now that you know the healthy baseline, here's what to watch for on the other side of the spectrum.
Redness and Color Changes
Inflamed gums turn red or dark red, especially along the gum margin and between teeth. In people with darker skin tones, inflammation may appear as a deepening of color or a shift toward purplish hues. The color change is caused by increased blood flow to the area as the body mounts an immune response against bacterial plaque.
Swelling and Puffiness
The gum tissue appears enlarged, rounded, or pillow-like rather than thin and firm. Swelling may be generalized (across many teeth) or localized (around one or two teeth). The tissue may look shiny or glossy due to stretching and loss of stippling.
Bleeding
As discussed above, any bleeding during brushing or flossing is a sign of inflammation. Some people dismiss this because it's been happening for so long they think it's normal. It isn't.
Recession
Gum recession means the tissue has pulled away from the tooth, exposing more of the tooth or its root. You may notice:
- Teeth that look longer than they used to
- Sensitivity to hot, cold, or sweet foods
- A visible notch or groove at the gum line
- Yellow or darker areas at the base of teeth (exposed root surface has a different color than enamel)
A 2018 population-based study in the Journal of Clinical Periodontology found that gum recession affects over 50% of adults, with prevalence increasing significantly after age 40.
Tenderness or Pain
Healthy gums are not painful. If your gums hurt when eating, brushing, or even at rest, something is wrong — whether it's gingivitis, periodontitis, an abscess, or another condition. Consult your dentist for evaluation.
Persistent Bad Breath
Chronic bad breath (halitosis) that doesn't improve with brushing, flossing, and tongue cleaning may indicate periodontal pockets where bacteria are producing volatile sulfur compounds. If this applies to you, our guide on how to get rid of bad breath permanently covers evidence-based solutions. Persistent halitosis is a common sign of moderate to advanced gum disease.
How to Do a Gum Self-Check at Home
You don't need any special equipment — just a mirror, good lighting, and clean hands. Try performing this check once a month.

Step 1: Look at the Color
Pull your lips and cheeks away from your teeth so you can see the gums around all your teeth, including the back molars. Note the overall color and look for any areas that are significantly redder or darker than the rest.
Step 2: Check the Texture
Look closely at the gums between your teeth and along the gum line. Are they stippled or smooth and shiny? Pay particular attention to areas that look swollen or glossy.
Step 3: Assess the Margins
Look at where each gum meets each tooth. Is the margin thin and tapered, or does it look thick, puffy, and rolled? Are the pointed papillae between teeth intact, or do you see dark gaps?
Step 4: Test for Bleeding
Brush your teeth normally, then floss. Note any areas that bleed. If bleeding occurs in the same spots consistently, those areas deserve closer attention from your dentist.
Step 5: Press Gently
Using a clean finger, press gently on the gums in various areas. They should feel firm, not spongy. They should not be painful to light pressure.
Step 6: Smell Check
Floss between your back teeth and smell the floss. A foul odor may suggest bacteria accumulating in pockets or between teeth where your brushing isn't reaching effectively.
How to Maintain the Gums You Want
If your self-check reveals healthy gums, congratulations — your job is to keep them that way. If you spotted some warning signs, the good news is that early gum disease (gingivitis) is reversible with consistent action.
Daily fundamentals:
- Brush twice daily for two minutes with a soft-bristled toothbrush
- Floss once daily (or use an interdental brush or water flosser)
- Clean your tongue — bacteria on the tongue contribute to both bad breath and gum disease
- Use a fluoride toothpaste
Supportive habits:
- Visit your dentist for cleanings at least twice per year (more often if you have a history of gum disease)
- Avoid tobacco in all forms — smoking is one of the strongest risk factors for periodontal disease, according to the American Academy of Periodontology
- Eat a balanced diet rich in vitamins C and D, both of which play roles in gum tissue maintenance and immune function
- Stay hydrated — adequate saliva production helps wash away bacteria and buffer acids in the mouth
Oral microbiome support:
Research over the past decade has increasingly shown that gum health isn't just about removing bad bacteria — it's about fostering a balanced oral microbiome. A 2021 review in Frontiers in Cellular and Infection Microbiology highlighted how dysbiosis (microbial imbalance) in the oral cavity is a driving factor in the shift from gum health to disease.

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim contains probiotic strains, including Lactobacillus reuteri and BLIS K-12, that research suggests may help support a balanced oral microbiome — one of the emerging pillars of long-term gum health.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
When Your Gums Don't Look Right: Next Steps
If your self-check revealed any warning signs — redness, bleeding, swelling, recession, or pain — don't panic, but don't ignore it either. Here's your action plan:
- Improve your oral hygiene immediately. The Loe experiment showed that gingivitis can develop in under three weeks of poor hygiene but also resolves when hygiene improves. Be consistent for at least two weeks before reassessing.
- Schedule a dental appointment. Only a professional exam with probing measurements and X-rays can tell you the full picture of your gum health.
- Consider your oral microbiome. If you've been using harsh antiseptic mouthwashes daily, you may be disrupting the beneficial bacteria that help keep your gums healthy.
Catching gum problems early is everything. Gingivitis is fully reversible. Once it progresses to periodontitis — with bone loss and deep pockets — the damage is managed rather than reversed. Learning to recognize the stages of tooth decay is equally important for catching problems before they become irreversible.

ProDentim
Oral Probiotic for Gum & Teeth Health
Maintaining the beneficial bacteria in your mouth may be just as important as removing the harmful ones. ProDentim delivers clinically studied probiotic strains that research suggests may help maintain the microbial balance associated with healthy gum tissue.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
Your Gums Are Telling You Something
Your gums are one of the most accessible windows into your oral health. Unlike bone loss or deep periodontal pockets — which require X-rays and clinical probing to detect — gum changes are visible to the naked eye. A monthly self-check takes less than five minutes and can alert you to problems months or even years before they become serious.
Learn what your personal "healthy baseline" looks like, and you'll know immediately when something changes. That awareness is one of the simplest, most powerful things you can do for your long-term dental health.
Related reading: