Several home remedies for gum inflammation have genuine research support. Saltwater rinses, turmeric, aloe vera, oil pulling, green tea, diluted hydrogen peroxide, cold compresses, and tea tree oil have all shown anti-inflammatory or antimicrobial effects in clinical studies. These remedies work best for mild gingivitis and as supplements to proper oral hygiene — they are not replacements for professional treatment when gum disease has progressed.
Swollen, red, bleeding gums aren't just uncomfortable — they're a signal that something needs attention. While professional dental care is essential for advanced gum disease, mild gum inflammation (gingivitis) often responds well to home remedies that are supported by actual research.
Here are eight options that have evidence behind them — not just internet folklore.
A Quick Note Before You Start
Home remedies work best when gum inflammation is mild — think redness, slight swelling, occasional bleeding when brushing. If you have deep pockets (4mm+), loose teeth, persistent bad breath, or gums that bleed heavily, you should consult your dentist before relying on home care alone. These may be signs of periodontitis, which requires professional treatment.
Also, no home remedy replaces the basics: brushing twice daily with proper technique and flossing every day. These remedies are add-ons, not substitutes.
1. Saltwater Rinse
The evidence: A saltwater rinse is the simplest and most time-tested home remedy for gum inflammation. A randomized controlled trial published in the Journal of Indian Society of Periodontology (2015) found that saltwater rinses reduced bacterial counts in the mouth and decreased gingival inflammation. The study found them comparable to chlorhexidine (a prescription-strength antiseptic mouthwash) for mild gingivitis.

Saltwater creates a hypertonic environment that draws fluid out of inflamed tissue through osmosis, reducing swelling. It also raises the oral pH, creating a less hospitable environment for acid-producing bacteria.
How to use it:
- Dissolve 1/2 teaspoon of table salt in 8 ounces of warm (not hot) water
- Swish gently for 30-60 seconds
- Spit out — don't swallow
- Repeat 2-3 times daily for 2-4 weeks
Pros: Cheap, accessible, virtually no side effects, safe for daily use. Cons: Won't reach below the gumline or remove tartar. Tastes unpleasant.
2. Turmeric Paste
The evidence: Curcumin, the active compound in turmeric, has well-documented anti-inflammatory properties. A meta-analysis published in the Journal of Indian Society of Periodontology (2020) analyzed multiple trials and found that curcumin-based mouthwashes and topical gels reduced plaque index and gingival inflammation scores comparably to chlorhexidine.
Curcumin works by inhibiting the NF-kB signaling pathway — one of the primary molecular switches that drives the inflammatory response in gum tissue. A study in Phytotherapy Research (2016) confirmed that curcumin reduced levels of IL-1beta and IL-6, two inflammatory cytokines directly involved in periodontal tissue destruction.
How to use it:
- Mix 1/2 teaspoon of turmeric powder with enough water or coconut oil to form a paste
- Apply directly to inflamed gums with a clean finger or soft brush
- Leave on for 10 minutes, then rinse thoroughly
- Use once daily
Alternatively, curcumin supplements (500mg daily with black pepper extract for absorption) provide systemic anti-inflammatory benefits that may support gum health from the inside.
Pros: Strong anti-inflammatory evidence, natural, affordable. Cons: Stains teeth and fabrics temporarily. Topical application can be messy.
3. Aloe Vera Gel
The evidence: Aloe vera contains compounds — including acemannan, aloin, and anthraquinones — that have anti-inflammatory, antimicrobial, and wound-healing properties. A study in the Journal of Clinical and Experimental Dentistry (2017) found that aloe vera gel, when used as an adjunct to brushing, significantly reduced plaque accumulation and gingival inflammation.

A separate study in the Journal of Indian Society of Periodontology (2016) compared aloe vera mouthwash to chlorhexidine and found comparable reduction in plaque and gingivitis scores over a 30-day period — without the side effects (staining, altered taste) associated with chlorhexidine.
How to use it:
- Use 100% pure aloe vera gel (food-grade, not the kind with added fragrances)
- Apply a small amount directly to inflamed gum areas
- Leave for 10 minutes, then rinse
- Repeat 2-3 times daily
- Alternatively, use an aloe vera-based dental gel or mouthwash
Pros: Soothing, anti-inflammatory, antimicrobial, promotes tissue healing. Cons: Must use pure aloe vera — many commercial products contain additives. Mild taste may be off-putting.
4. Oil Pulling
The evidence: Oil pulling — swishing oil in the mouth for an extended period — is an ancient Ayurvedic practice that has attracted modern research attention. A systematic review in the Journal of Traditional and Complementary Medicine (2020) found that oil pulling with coconut or sesame oil reduced plaque and gingivitis scores comparably to chlorhexidine mouthwash across multiple trials.
The proposed mechanism is that the oil's lipid layer attracts and binds lipid-coated bacteria (including periodontal pathogens), physically removing them from the oral cavity. Coconut oil specifically contains lauric acid, which has demonstrated antimicrobial activity against Streptococcus mutans and other oral bacteria in laboratory studies (Nigerian Journal of Medicine, 2015).
How to use it:
- Place 1 tablespoon of organic coconut oil in your mouth
- Swish gently (don't gargle) for 15-20 minutes
- Spit into the trash — not the sink (oil can clog pipes)
- Do not swallow the oil
- Brush your teeth afterward
- Best done in the morning before eating
Pros: Well-studied among traditional remedies, reduces bacterial load, no side effects. Cons: Time-consuming (15-20 minutes). Cannot reach subgingival bacteria. Does not remove tartar.
5. Green Tea
The evidence: Green tea contains catechins — particularly epigallocatechin gallate (EGCG) — that have both anti-inflammatory and antimicrobial properties specific to oral health. A study in Archives of Oral Biology (2016) found that EGCG inhibited the growth of P. gingivalis, one of the primary bacteria responsible for periodontal disease.
A population study published in the Journal of Periodontology (2009) followed over 900 men and found that those who regularly consumed green tea had significantly lower periodontal pocket depths, less clinical attachment loss, and less gum bleeding than non-drinkers. The benefit increased with consumption — those drinking 3+ cups daily showed the strongest protective effect.
How to use it:
- Drink 2-3 cups of unsweetened green tea daily
- For topical benefit, swish cooled green tea in your mouth for 30 seconds before swallowing
- Or apply a cooled green tea bag directly to inflamed gum areas for 5-10 minutes
- Avoid adding sugar, which would counteract the benefit
Pros: Enjoyable, systemic anti-inflammatory benefits, strong epidemiological evidence, antioxidant-rich. Cons: Can stain teeth with heavy use. Caffeine may be an issue for some.
6. Diluted Hydrogen Peroxide Rinse
The evidence: Hydrogen peroxide has been used as an oral antiseptic for over a century. At appropriate concentrations, it reduces bacterial load and may help control gum inflammation. A study in the Journal of Clinical Periodontology (2004) found that a 1% hydrogen peroxide rinse reduced gingival bleeding when used as an adjunct to mechanical cleaning.
The American Dental Association considers hydrogen peroxide rinses safe for short-term oral use when properly diluted.
How to use it:
- Mix equal parts 3% hydrogen peroxide (standard pharmacy concentration) and water, creating a 1.5% solution
- Swish for 30-60 seconds
- Spit out completely — do not swallow
- Use 2-3 times per week (not daily, as prolonged use may irritate soft tissue)
- Do not use undiluted hydrogen peroxide in the mouth
Pros: Strong antiseptic, widely available, inexpensive. Cons: Can irritate tissue if used too frequently or at too high a concentration. Damages healthy tissue at higher concentrations. May cause foaming that some find unpleasant. Short-term use only.
Important: If you have deep periodontal pockets, hydrogen peroxide rinses should only be used under dental guidance, as the solution may trap oxygen in pockets and cause tissue damage. Similarly, be aware that some antiseptic mouthwashes can kill beneficial bacteria and may do more harm than good when overused.
7. Cold Compress
The evidence: While not a treatment for the underlying infection, cold application reduces acute gum inflammation and pain through vasoconstriction — narrowing of blood vessels that decreases blood flow to the area, reducing swelling. This is basic physiology supported by decades of clinical use for soft tissue inflammation (Clinical Oral Investigations, 2015).
A cold compress is most useful for acute episodes of gum pain and swelling — after dental procedures, during a flare-up, or when gum inflammation is causing significant discomfort.
How to use it:
- Wrap ice or a gel pack in a thin cloth (never apply ice directly to skin or gums)
- Apply to the outside of the cheek over the affected area
- Hold for 15-20 minutes, then remove for 15-20 minutes
- Repeat as needed
- For direct gum application, hold a small ice chip against the inflamed area briefly (10-15 seconds)
Pros: Immediate pain and swelling relief, no side effects, universally accessible. Cons: Addresses symptoms, not the cause. Temporary relief only. Not effective for chronic inflammation.
8. Tea Tree Oil (Diluted)
The evidence: Tea tree oil (melaleuca) has demonstrated antimicrobial activity against a range of oral pathogens in laboratory settings. A study in the Australian Dental Journal (2008) found that a tea tree oil gel reduced gingival bleeding and inflammation scores when applied topically to inflamed gums. A study in Oral Microbiology and Immunology (2003) showed that tea tree oil inhibited P. gingivalis, Prevotella intermedia, and Fusobacterium nucleatum — three key periodontal pathogens.
How to use it:
- Never use undiluted tea tree oil in the mouth — it is too concentrated and can cause chemical burns
- Add 2-3 drops of tea tree oil to 8 ounces of warm water as a rinse
- Or add 1 drop to your toothpaste before brushing
- Or look for dental products that already contain tea tree oil at appropriate concentrations
- Use once daily for no more than 4 weeks
Pros: Antimicrobial against key periodontal pathogens, available as commercial dental products. Cons: Must be properly diluted — toxic if swallowed in significant quantities. Can cause allergic reactions in some individuals. Unpleasant taste. Not as well-studied as some other remedies on this list.
Combining Remedies: A Practical Daily Routine
You don't need to use all eight remedies. Here's a practical combination for managing mild gum inflammation at home:
Morning:
- Oil pulling with coconut oil for 15-20 minutes (while getting ready)
- Brush with Modified Bass technique (soft brush, 45-degree angle, 2 minutes)
- Floss
- Drink green tea with breakfast
After lunch:
- Saltwater rinse (30-60 seconds)
Evening:
- Brush thoroughly
- Floss
- Apply aloe vera gel or turmeric paste to inflamed areas (10 minutes, then rinse)
2-3 times per week:
- Diluted hydrogen peroxide rinse
As needed:
- Cold compress for acute swelling or pain
Supporting Your Oral Microbiome
Beyond these topical remedies, supporting the overall balance of bacteria in your mouth may help reduce inflammation at its source. Oral probiotics — particularly strains like Lactobacillus reuteri — have been shown in clinical trials to reduce gingival bleeding and inflammation when used alongside regular oral hygiene.
A systematic review in the Journal of Clinical Periodontology (2020) found that probiotic supplementation as an adjunct to standard care improved clinical outcomes including reduced bleeding on probing and pocket depth. The theory: when beneficial bacteria occupy the ecological niches in your mouth, pathogenic species have less room to establish themselves. Your diet also plays a major role in shaping this microbial balance.

ProDentim
Oral Probiotic for Gum & Teeth Health
ProDentim delivers 3.5 billion CFU of targeted oral probiotic strains, including L. reuteri, in a dissolving tablet designed to colonize the oral cavity. Research suggests these strains may reduce gum inflammation and support a healthier bacterial balance in the mouth.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
When Home Remedies Aren't Enough
Home remedies have real limits. Consult your dentist if:
- Bleeding persists for more than 2-3 weeks despite consistent home care improvements
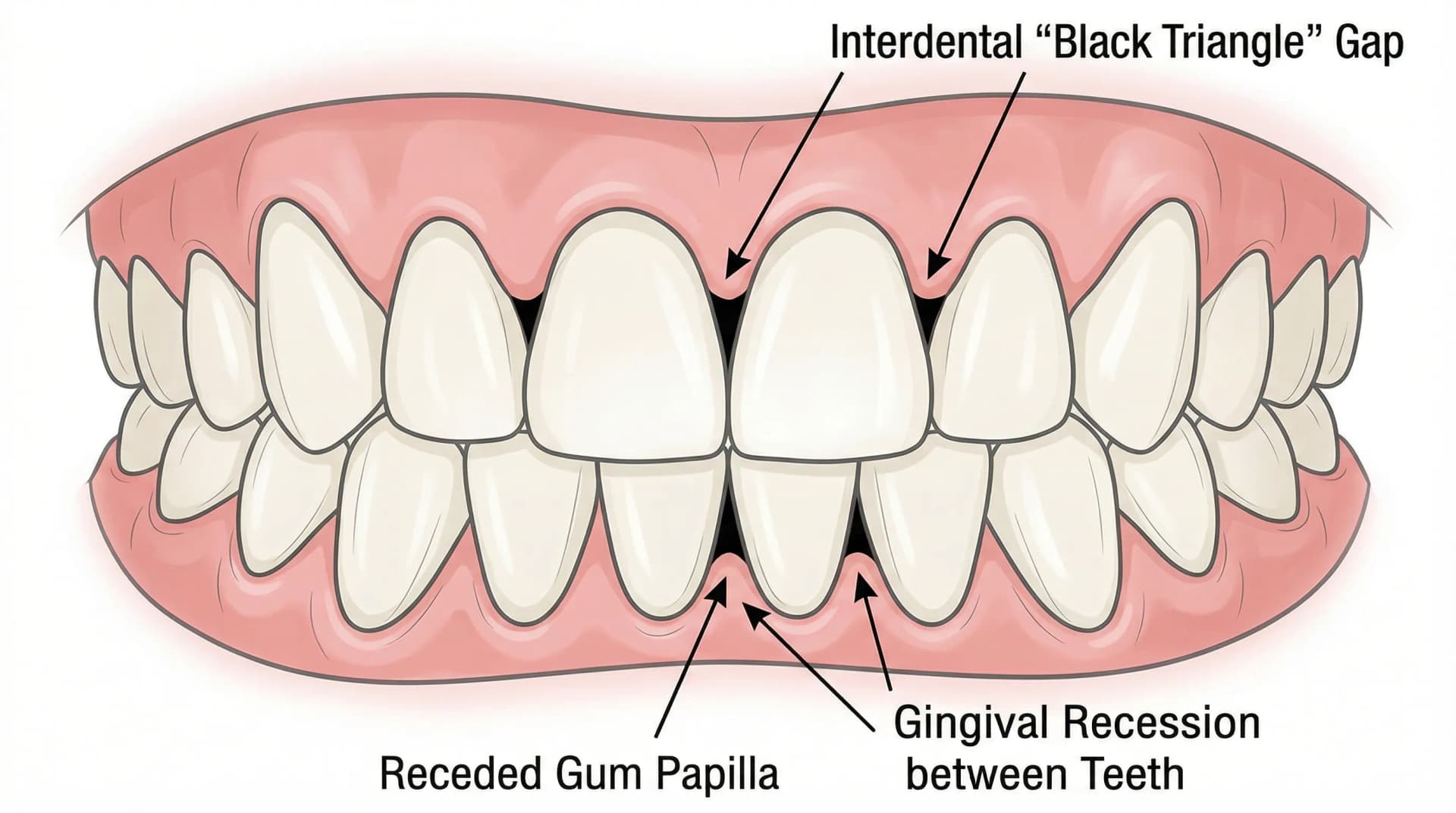
- Gums are pulling away from teeth (visible recession)
- You have persistent bad breath that doesn't improve with better hygiene
- Teeth feel loose or have shifted position
- You see pus between teeth and gums
- Pain is severe or you have fever (possible dental abscess — seek care immediately)
- Pocket depths measure 4mm or deeper at your last dental visit
These signs may indicate periodontitis — a condition that requires professional scaling and root planing, not just home remedies. Using home remedies to avoid dental treatment for advancing gum disease is a recipe for tooth loss.
The Role of Prevention
The best home remedy for gum inflammation is preventing it in the first place. The vast majority of gingivitis cases result from inadequate plaque removal — and the fix is mechanical, not chemical. A study in the Journal of Clinical Periodontology (2015) found that effective plaque removal alone resolved gingivitis in 95% of cases within 4 weeks.
No rinse, gel, supplement, or paste can compensate for poor brushing and flossing. These remedies are valuable additions to a solid foundation — but the foundation has to be there first.

ProDentim
Oral Probiotic for Gum & Teeth Health
Adding a targeted oral probiotic like ProDentim to your daily routine may help maintain the microbial balance that supports healthy, inflammation-free gums — especially when combined with proper brushing, flossing, and the home remedies outlined above.
We may earn a commission if you make a purchase through our links, at no extra cost to you.
Take care of the basics, use these research-backed remedies as your supporting cast, and you'll give your gums the best chance to stay healthy — or return to health if mild inflammation has already set in.
Related reading: